Endocarditis – A Complicated Case
- Nov 27th, 2014
- Whitney Lewis
- categories:
Endocarditis: A Complicated Case
By Whitney Lewis DO
Senior EM Resident, UTSW/Parkland
Edited by Walter Green MD, Alex Koyfman MD, and Stephen Alerhand MD
CC: Chest pain and shortness of breath
HPI: 37-year-old male with PMH significant for Type II DM and chronic non-healing bilateral forearm wounds presented to the emergency department with chest pain described as a sub-sternal, non-radiating, pressure-like pain that was constant for three days, with associated dyspnea on exertion, orthopnea, and fever. The chest pain was exacerbated by activity and deep breathing with no stated alleviating factors. Additionally, the patient noted a recent history of constant LUQ sharp abdominal pain with associated nausea, non-bloody diarrhea, and decreased appetite. The patient also reported that the chronic bilateral forearm wounds appeared one year ago as “small spots” and had progressively increased in size. The lesions were non-tender, did not itch or burn, and per the patient were healing with the administration of Neosporin and alcohol. The patient denied previous cardiac problems, surgeries, or history of inflammatory bowel disease. The patient had not obtained prior medical care for the forearm wounds and the patient denied previous incidents of similar skin lesions, trauma, IVDA, or burns. Of note, the patient made mention of recent vision blurriness, trouble with word finding, and decreased concentration, but denied headaches, new sensation changes, or focal weakness.
PE: Pertinent physical exam findings included an afebrile, obese male with poor dentition who was tachycardic without an audible murmur, gallop, or rub, and demonstrated minimal tenderness to palpation in the LUQ of the abdomen with voluntary guarding. Two large irregularly shaped ulcers were present on the dorsal forearms; the left upper extremity demonstrated a 13 cm x 8 cm area of granulation tissue and the right upper extremity a 7 cm x 7 cm area of granulation tissue. Both wounds featured exposed muscle fibers and tendons covered by a dry yellow crust. The edges of the lesions were brown, sharply demarcated, non-erythematous, and firm. The patient demonstrated an odd, flat affect but was otherwise neurologically intact.
Labs: Lipase 129, CRP 1.5, ESR 37, HgbA1c 8.7, Hgb/HCT 11.7/35.8, MCV 67, two consecutive troponin T values were negative.
Imaging: Bilateral forearm x-rays revealed large soft tissue ulcers and soft tissue swelling in the region of the wounds. CXR showed a RLL granuloma.
EKG: Sinus tachycardia with LVH.
Visual acuity: R eye 20/20 and L eye 20/25.
The patient was given an aspirin, placed on broad-spectrum antibiotics, and reluctantly admitted by the Hospitalist for continued work-up. The patient subsequently developed L eye pain with vision loss prompting further diagnostic imaging. A CT and MRI of the head were obtained and demonstrated multiple ring-enhancing lesions in the bilateral cerebral hemispheres, predominately within the left frontal, parietal, and occipital lobes. The largest lesion, in the left frontal lobe, measured 5.3 x 3.3 x 4.2 cm, the findings were suggestive of multiple brain abscesses.
What further imaging modalities should be acquired? What is the diagnosis?
- Echocardiography (TTE and/or TEE): normal LV systolic function, LVEF 71%, a large vegetation present on the aortic valve with mild to moderate aortic insufficiency.
- CT abdomen and pelvis: hepatosplenomegaly with large devascularized areas in the spleen consistent with infarcts.
Diagnosis: Aortic valve endocarditis complicated by septic emboli to the brain and spleen
Extended hospital course: Blood and forearm cultures grew Methicillin-sensitive Staphylococcus aureus (MSSA). On day 5 of the patient’s hospitalization, Neurosurgery completed a left frontal craniotomy in order to access, culture, and wash-out the largest intracranial abscess. The abscess cultures grew MSSA. The patient then underwent dental clearance and teeth extraction by Oral Maxillofacial surgery prior to Cardiothoracic surgery placing an aortic mechanical valve. Regarding the chronic non-healing forearm ulcers, Dermatology completed punch biopsies of both lesions with findings consistent with the injection of foreign material into the skin. Ultimately, the patient recovered without complications and completed a six-week course of Nafcillin.
Infective endocarditis (IE):
- Definition – an infection of the valves or lining of the heart, most commonly caused by bacteria.
- Bacteremia occurs when organisms enter the bloodstream through the lining of the mouth or intestine, or through skin cuts, abrasions, or breakdown.
- Prosthetic heart valves, rheumatic or congenital heart diseases, pacemakers, invasive procedures, and the use of intravenous self-administered illicit drugs may predispose a susceptible person to developing bacteremia and put them at an increased risk of acquiring endocarditis.
- Presenting signs and symptoms: fever, loss of appetite, unexplained weight loss, new skin lesions (Osler nodes and Janeway lesions), splinter hemorrhages, headache, joint pain, confusion, shortness of breath, heart murmur, fatigue, or sudden weakness in the face or limbs.
- Duke criteria for IE:
- Major criteria include 2 positive blood cultures with microorganisms consistent with IE or evidence of endocardial involvement (intracardiac mass, abscess, or new valvular regurgitation).
- Minor criteria include predisposing condition (heart condition, IVDA), fever, vascular phenomenon (emboli, skin lesions), immunologic phenomenon (Osler’s nodes, Roth spots), microbiological evidence, ECHO findings concerning for IE
- (Editor’s note: BE FEVEER mnemonic: Major – Blood culture + >2x 12 hrs apart, Endocardial involvement from echo; Minor – Fever, Echo findings, Vascular findings, Evidences from microbiology/immunology, Risk factors such as drug abuse or valvular disease)
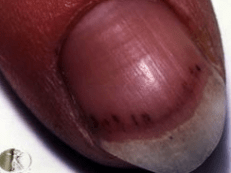
- (Editor’s note: FROM JANE mnemonic: Fever, Roth spots, Osler nodes, Murmur, Janeway lesions, Anemia, Nail-bed Hemorrhage, Emboli)
- Complications: destruction of heart valves, congestive heart failure, and/or embolic complications that can lead to organ damage, brain abscesses and infarcts.
- Acute IE: patients are younger, most common cause => Staphylococcus aureus, carries a higher morbidity and mortality rate than subacute IE.
- Subacute IE: patients are older with abnormal valves and most common cause is Streptococcus viridans.
- Treatment includes antimicrobial therapy for 4 to 6 weeks and surgery, when clinically indicated, to repair damaged heart valves or remove infected tissue from the brain.
- Surgical indications: refractory CHF, valve ring abscess, multiple major emboli, medical failure, and/or mycotic aneurysm.
References
– Cabell, Christopher H., Elias Abrutyn, and Adolf W. Karchmer. “Bacterial Endocarditis The Disease, Treatment, and Prevention.” Circulation 107.20 (2003): e185-e187.
– Li, Jennifer S., et al. “Proposed modifications to the Duke criteria for the diagnosis of infective endocarditis.” Clinical infectious diseases 30.4 (2000): 633-638.
– Millar BC, Moore JE. Emerging issues in infective endocarditis. Emerg Infect Dis [serial on the Internet]. 2004 Jun [date cited]. Available from: http://wwwnc.cdc.gov/eid/article/10/6/03-0848.htm
– Pao-Tsuam Kao, et al. Brain abscess: clinical analysis of 53 cases. Division of Infectious Diseases, Department of Internal Medicine, Mackay Memorial Hospital, Taipei, Taiwan, ROC. Journal of Microbiology Immunology Infect, 2003; 36; 129-136.
– http://www.ncbi.nlm.nih.gov/pubmed/24079983
– http://www.ncbi.nlm.nih.gov/pubmed/23399454
– http://www.ncbi.nlm.nih.gov/pubmed/25215124
– http://www.ncbi.nlm.nih.gov/pubmed/21763096
– http://www.ncbi.nlm.nih.gov/pubmed/22461931






2 thoughts on “Endocarditis – A Complicated Case”