#1: Peripheral Pressors – Complications in a Meta-Analysis
Spoon Feed
In this systematic review and meta-analysis, there was a very low prevalence of complications related to vasopressor infusion through a peripheral IV, and using at least a 20-gauge catheter seems to make it safer for patients.
Why does this matter?
Delayed initiation of vasopressors is associated with increased mortality. In one study of 8,670 patients, each hour of delay was associated with a 2% increase in in-hospital mortality. If we can safely initiate vasopressor infusion through peripheral venous catheters, we have the opportunity to impact patient care. We reviewed a large retrospective study of peripheral pressors in the past. What’s the consensus?
Can we safely start it?
Nine studies were included in this systematic review and meta-analysis which included a total of 1,835 patients – the clinical setting for two of these studies was exclusively in the ED and exclusively administered through peripheral venous catheters. The seven remaining studies were performed in the ICU setting. The most common catheter size was a 20-gauge, and the most common vasopressor was norepinephrine. The maximum dose of norepinephrine was 0.13mcg/kg/min. There were 122 complications in total (7%) – of which 117 (96%) were classified as minor complications (infiltration, erythema) and 5 (4%) were classified as a major complication (peripheral venous thrombosis). However, most studies reported no required treatment for the complication. Unfortunately, the authors of this study did not identify patient demographics or clinical factors that would potentially predict a higher risk of complications. Interestingly, the meta-analysis revealed a trend toward much lower rates of complications in studies performed after 2016 (5% complication rate) as opposed to those before 2010 (25% complication rate), likely due to the use of point-of-care ultrasound used to confirm proper placement. No question – I would start vasopressors peripherally in the ED for shock as opposed to administering more fluid if your patient has been adequately volume resuscitated.
Source
Complication of vasopressor infusion through peripheral venous catheter: A systematic review and meta-analysis. Am J Emerg Med. 2020 Sep 28;S0735-6757(20)30842-1. doi: 10.1016/j.ajem.2020.09.047. Online ahead of print.
Open in Read by QxMD
#2: Topical Tetracaine for Corneal Abrasions
Spoon Feed
Short-term use of topical tetracaine for uncomplicated corneal abrasions was associated with significant pain reduction and decreased need for opioid medications, with no difference in wound healing or serious complications. However, larger studies are needed to definitively demonstrate safety and rule out rare adverse events.
Why does this matter?
Corneal abrasions are the most common ocular injuries encountered in the acute care setting. Most corneal abrasions heal spontaneously within 24 to 72 hours, but they are particularly painful, and adequate analgesia can be a real problem. Discharging patients with topical anesthetic agents such as tetracaine or proparacaine can provide excellent analgesia but has historically been avoided due to concerns for poor wound healing and subsequent corneal ulceration, scarring, or blindness.
However, evidence for the harmful effects of topical anesthetics is limited and comes from case reports, case series, and animal studies, many of which included high concentrations and long-term use of topical agents. So, is this dogma justified, or can topical anesthetics be a useful tool to treat the severe pain associated with corneal abrasions?
You’ll melt your eye out…or will you?
This was a prospective, randomized, double-blind, placebo-controlled trial of 111 patients comparing patient home use of topical tetracaine 0.5% (1 drop every 30 minutes as needed for a maximum of 24 hours) vs placebo (artificial tears) for uncomplicated corneal abrasions.
Topical tetracaine use was associated with lower median pain score (1/10 vs 8/10) and decreased use of hydrocodone tablets for breakthrough pain (median 1 vs 7) compared to placebo for the first 24 to 48 hours. No serious adverse events were reported, and there was no significant difference in the rate of complications or residual corneal abrasions noted at the 24- to 48-hour follow up visits. Of note, there were numerous exclusion criteria, and only patients with uncomplicated corneal abrasions were included. In addition, this was a small, single center study, and it was not powered to establish safety or rule out rare adverse events.
Based on this data, short-term use of topical tetracaine for up to 24 hours appears to be both efficacious and relatively safe. However, the overall safety profile and rate of rare adverse events is still unknown. Therefore, before you send patients home with topical tetracaine for corneal abrasions, counsel them on the correct use of topical anesthetic agents and on the potential risks of abuse/misuse. Patients discharged with topical anesthetics should also be given strict return precautions along with instructions for close ophthalmology follow-up.
Another Spoonful
These resources take an in depth look and literature review of topical anesthetics for corneal abrasion.
Source
Short-Term Topical Tetracaine Is Highly Efficacious for the Treatment of Pain Caused by Corneal Abrasions: A Double-Blind, Randomized Clinical Trial. Ann Emerg Med. 2020 Oct 27;S0196-0644(20)30739-3. doi: 10.1016/j.annemergmed.2020.08.036. Online ahead of print.
Open in Read by QxMD
#3: Diagnosis and Management of DVT – Spoon-Feed Version
Spoon Feed
This article reviews recent literature investigating the diagnosis and management of lower extremity DVT.
Why does this matter?
We see patients with LE DVT frequently, and the management of this disease continues to evolve. Here is a summary of the latest information you need to know.
Did I develop a DVT from too much turkey?
In this systematic review, authors siphoned through 2,100 articles produced over the last five years, developing a practice-changing brief of RCTs, meta-analyses, observational studies, and guidelines.
Epidemiology
-
An isolated distal (i.e. calf vein) DVT carries an all-cause mortality rate of 4.6 per 100 person years.
-
Risk factors for DVT include obesity, pregnancy, malignancy, major surgery or immobilization, CKD, atherosclerosis, diabetes, infection, inflammatory disease, chronic lung disease, heart failure and inherited disorders.
Diagnosis
-
Pretest probability or D-dimer do not rule out DVT by themselves; they should be used together.
-
Use a Wells score to categorize your patient as high or low risk. The Wells score does not perform well for inpatients.
-
If low or moderate risk (i.e. Wells <3), use age adjusted D-dimer to stratify further. Wells <3, high-sensitivity D-dimer negative, rules our DVT. Any positive D-dimer warrants ultrasound.
-
If high risk (i.e. Wells ≥3) or in cancer patients, skip the D-dimer and go straight to ultrasound.
-
Negative two-point compression ultrasounds need a repeat scan in 5-7 days. Whole-leg US is usually preferred.
-
Be aware of other diagnoses such as May-Thurner Syndrome, superficial thrombophlebitis, and post-thrombotic syndrome.
Treatment
-
DOACs are non-inferior to warfarin and cause less bleeding.
-
The largest barrier to DOACs is cost.
-
Use LMWH with pregnancy and malignancy; however, DOACs may be used in non-gastrointestinal malignancy.
-
Most patients with good follow-up can be managed as an outpatient.
-
Aspirin for secondary prevention has higher rates of recurrence than DOACs.
-
Treat isolated calf vein DVT if, “severe symptoms or risk factors for pulmonary embolism or extension to proximal veins (such as hospitalization, history of VTE, and cancer.”
-
Catheter-directed thrombolysis does not reduce recurrence of DVT, post-thrombotic syndrome, and may increase bleeding.
Next is a handy table to decide on the right treatment modality, and an algorithm proposed by the authors to put this all together.
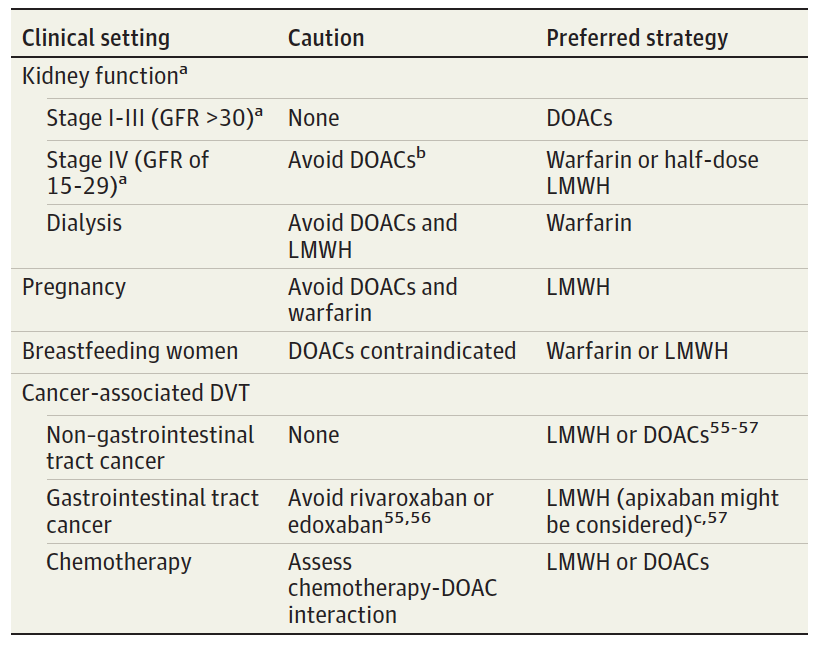
From cited article
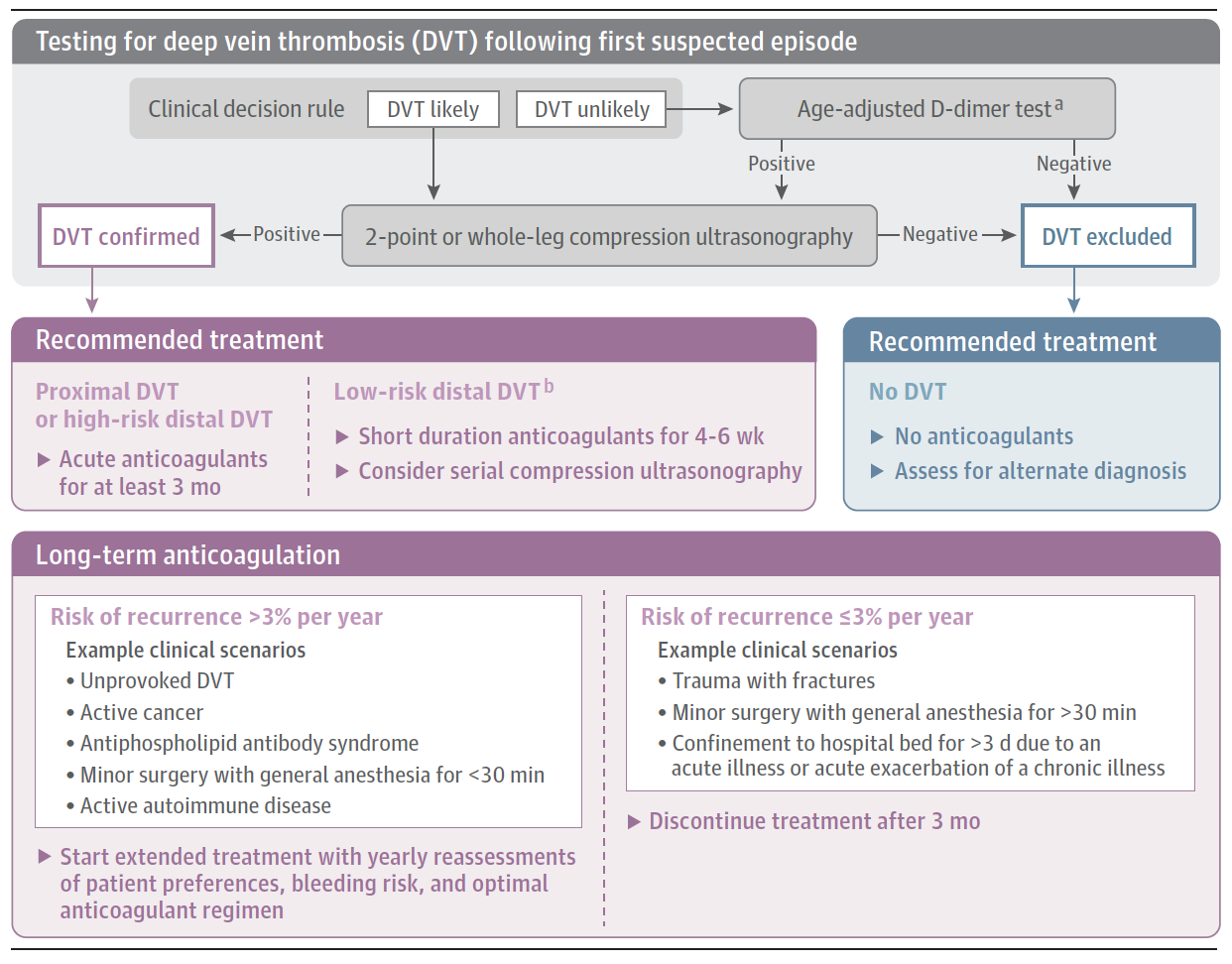
From cited article with these disclaimers:
“This algorithm has not been validated in clinical trials but represents a synthesis of evidence-based approaches to DVT diagnosis and management.
a Age-adjusted D-dimer threshold, calculated as the patient’s age multiplied by 10 ng/mL for patients older than 50 years with suspected venous thromboembolism.
b Low-risk patients: younger than 50 years, no cancer or prior venous thromboembolism, taking contraceptive or replacement hormonal therapy, and secondary to surgery or immobilization when complete mobilization is achieved.”
Source
Diagnosis and Treatment of Lower Extremity Venous Thromboembolism: A Review. JAMA. 2020 Nov 3;324(17):1765-1776. doi: 10.1001/jama.2020.17272.
Open in Read by QxMD





