Today on the emDocs cast with Brit Long, MD (@long_brit) and Manpreet Singh, MD (@MprizzleER) we cover wounds and lacerations in the ED.
Episode 23: Wounds and Lacerations
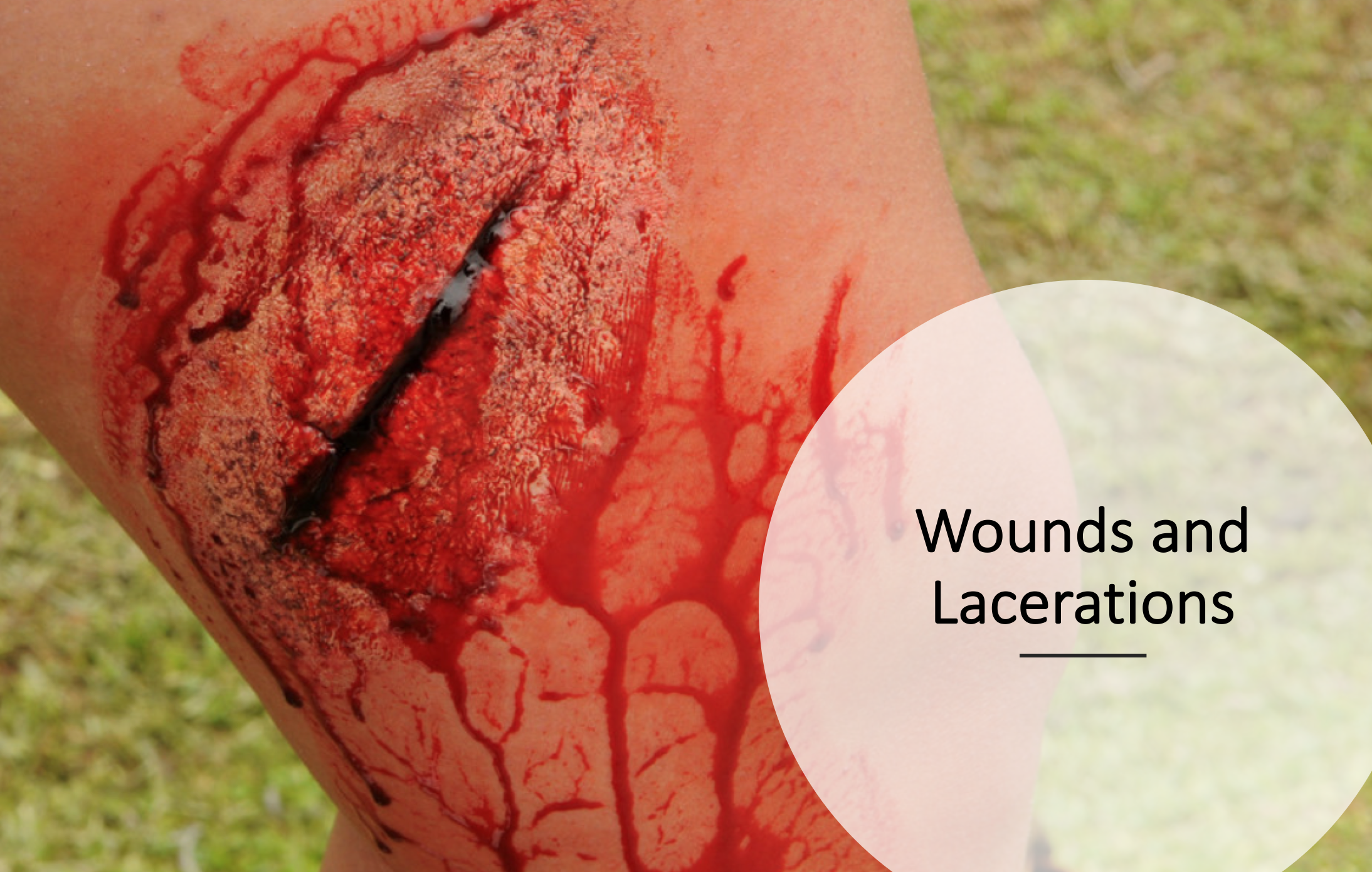
– Lacerations and acute wounds account for approximately 9 million visits annually.
– Wounds require appropriate physical evaluation for extent of injury, radiographic evaluation for secondary injury, and irrigation & exploration for wound cleansing with removal of foreign body and debris.
Key Questions:
- What emergent diagnoses should you consider in this patient?
- What’s the neurovasular status?
- What additional diagnostic testing should be considered in a wound close to a joint?
- What are some factors that make this wound high risk for infection, and is tetanus up to date?
- Could a foreign body be present?
Pathophysiology: The pathway to healing occurs in sequential fashion; briefly summarized by a hemostatic phase which includes platelet aggregation and clot formation, a proliferative phase mediated by leukocytes, and the maturation and remodeling phases that gradually improve wound tensile strength and integrity. Any breaks in this progress alters healing.
Evaluation: mechanism of injury, location, and length of injury, as well as the degree of contamination, time since injury, tetanus vaccination status, and any neurovascular or musculoskeletal deficits.
- If the mechanism of injury, location, depth, or deficits in movement/sensation is concerning for nonvisualized retained foreign body, bone involvement, joint involvement, compartment syndrome, or neurovascular injury, then advanced imaging would be most useful to ensure full evaluation of the extent of injury.
- Imaging options include Xray, CT, and US.
- Evaluate tetanus history and update as needed. Evaluate comorbidities.
Management: Clean vs. dirty wounds.
- Removal of gross contamination of dirt, debris, foreign bodies as well as bacterial load begins with wound irrigation.
- Irrigate – Tap water is safe. Earlier is better. Amount of irrigation is most important (50-100cc per 1 cm wound). Avoid excess pressure; aim for 5-13 psi.
Types of closure: primary (immediate fixation), delayed primary (delay in wound closure to allow for evaluation at a later date), secondary intention (wound heals by contraction)
Anesthesia: Ester or amid anesthetics disrupt sensory nerve conduction. Other options for local anesthesia can include topical lidocaine-epinephrine-tetracaine (LET), benadryl, or ketamine.
Closure materials: Sutures, staples, adhesive tape, tissue adhesive. Each has positives, negatives, prime situations.
Wounds sites: All have important specific considerations –> scalp (galea), forehead (muscle repair for function), eyelids (location is key), ears (cartilage), lip (vermillion border), arm/hand (neuromuscular injury), fist fight injuries (do not suture, provide antibiotics), flexor tendon/volar injuries, extensor tendon/dorsal injuries, fingertips/nails (amputation, nail bed), leg/foot.
Can’t Miss Injuries: open fracture, open joint, compartment syndrome, tendon injury, arterial injury/compromised vasculature, foreign body, nerve/muscle injury, human bite.
- Open Fracture > visual inspection, Xray/CT; needs immediate antibiotics (first generation cephalosporin, add gentamicin if heavily contaminated), washout with orthopedics/trauma.
- Open Joint > confirm with Xray/CT; needs immediate antibiotics (again, first generation cephalosporin, add gentamicin if heavily contaminated), washout with orthopedics/trauma.
- Compartment Syndrome > confirm with physical exam/suspicion; needs immediate fasciotomy/OR management.
- Tendon injury > confirm with physical exam, CT scan; repair (if visible), splint and follow up with specialist vs specialist consultation.
- Arterial injury/compromised vasculature > confirm with inspection, CT; control bleeding, vascular/specialist surgical consultation in ED.
- Foreign body > visual inspection, Xray/CT/Ultrasound imaging; not all require removal if search risks damage to surrounding structures; small, inert, deep or asymptomatic foreign bodies can potentially stay; remove all reactive or contaminated foreign (thorns, wood, spines) immediately if possible.
- Nerve injury > physical examination; assess before and after repair, needs specialist follow up for prolonged recovery monitoring.
- Muscle injury > physical examination, CT imaging; needs repair to recover function, splint in functional position and follow up with specialist.
- Human bite > history/visual inspection; always needs antibiotics, needs wound check follow up.







1 thought on “emDOCs Podcast – Episode 23: Wounds and Lacerations”
Pingback: REBEL Core Cast 56.0 - Wound Care III - Pitfalls - REBEL EM - Emergency Medicine Blog