Authors: Skyler Lentz, MD (@skylerlentz, Critical Care Fellow and Instructor in Medicine, Dartmouth-Hitchcock Medical Center) and Matthew Roginski, MD, MPH (@mattroginski, Assistant Professor of Medicine, DHART Assistant Medical Director, Dartmouth-Hitchcock Medical Center) // Editors: Alex Koyfman, MD (@EMHighAK) and Brit Long, MD (@long_brit)
Case
An 85-year-old female with dementia and dysphagia presents to the emergency department with progressive hypoxia after her health aid witnessed an aspiration event with dinner last night. This morning she was more lethargic which prompted a call to EMS who recorded a room air saturation of 78% that required a non-rebreather to bring the SpO2 >92%. On exam she is confused from her baseline, mildly tachypneic on a non-rebreather with rales in the right mid and lower lung zones. Portable chest x-ray shows a new haziness on the right. The patient is unable to answer questions, family is on the way, and there are no advanced directives with the patient. Should you keep her on a non-rebreather mask, try non-invasive positive pressure ventilation, or initiate high-flow nasal cannula?
What is a high-flow nasal cannula?
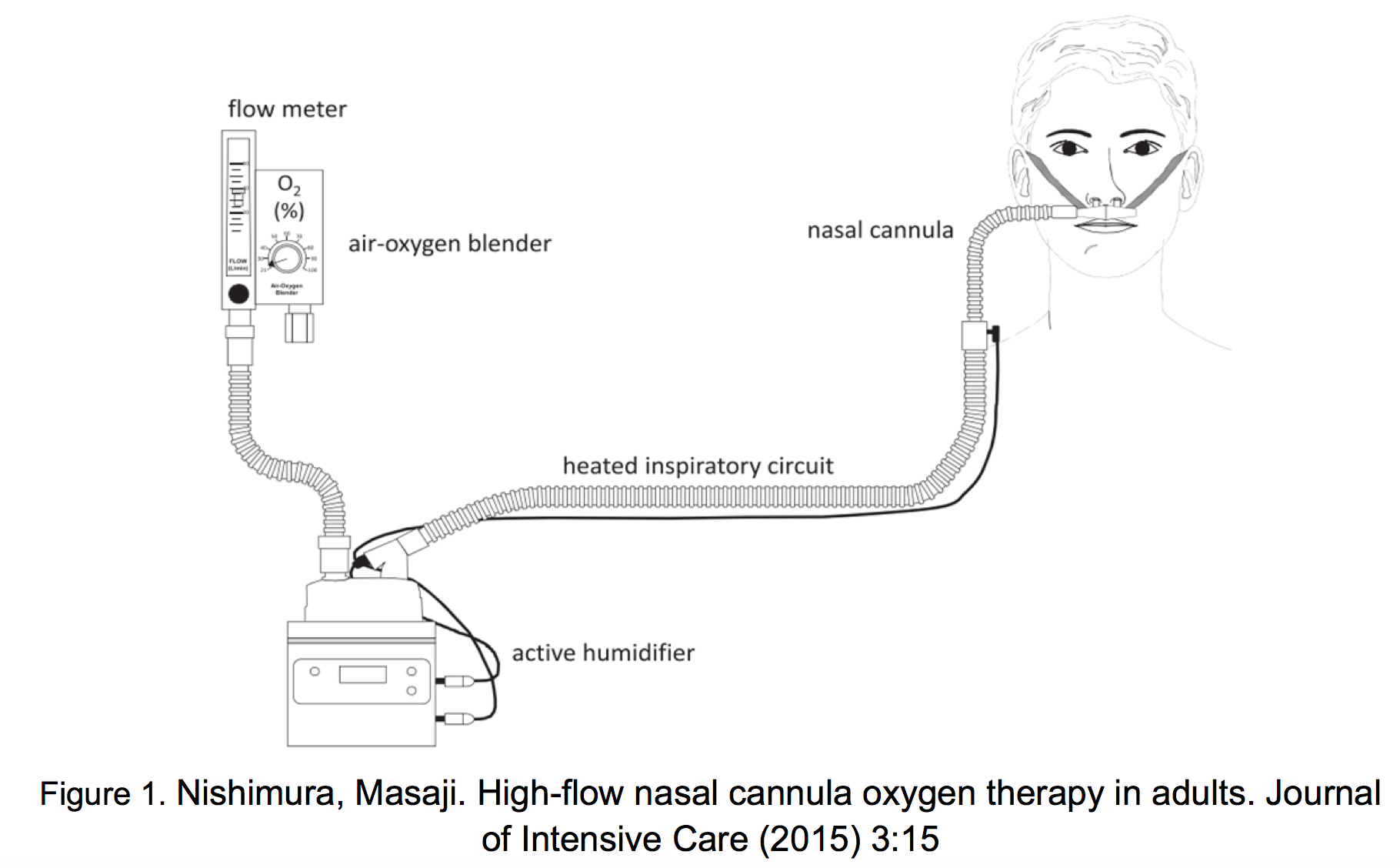
The high flow nasal cannula (HFNC) is a special device that can deliver a continuous flow of gas between 20 and 60 L/min and offers many physiologic advantages that other oxygen delivery systems do not [1,2]. As seen in figure 1, HFNC requires specific devices, (i.e. OptiFlow™, Vapotherm etc.) which blend compressed medical air and oxygen to deliver a continuous flow of 20-60 L/min through a warmed and humidified circuit. HFNC devices typically require respiratory therapists or specially trained nurses for set-up, but once set-up in the ED, emergency physicians will need to manage HFNC titration (see “Prescribing HNFC in the ED” below). If resources allow, HFNC can be a first-line therapy in patients with hypoxemic respiratory failure not from cardiogenic pulmonary edema and without concomitant hypercapnia [1].
HFNC is a special device that uses a large bore nasal cannula to deliver 20-60 L/min of a warmed and humidified blend of oxygen and medical air.
How does it work? It’s the Flow.
HFNC washes out nasopharyngeal dead space, improves oxygenation, decreases the work of breathing and respiratory rate, generates a low level of positive airway pressure, and provides heated and humidified gas to promote secretion clearance. The high flow rate makes breathing more efficient because it washes out the dead space. When a patient is in distress, the wash out of dead space makes breathing more efficient because it significantly decreases the amount of re-breathed carbon dioxide and acts as a continuous reservoir of new gas. This ultimately decreases the respiratory rate and work of breathing in your patient [1,2].
The flow washes out the dead space of the upper airway and reduces the work of breathing.
While HFNC can deliver high rates of continuous oxygen flow, it does not provide a titratable pressure like NIPPV (i.e. BiPAP and CPAP). HFNC can deliver low level positive pressure to the upper airways in the range of 2-5 cm H2O. The actual pressure depends on the flow rate, patient’s mouth being open or closed (higher with mouth closed), and phase of the respiratory cycle (higher pressures during exhalation) [4,5].Even these low levels of upper airway pressure can increase the functional residual capacity (FRC) and lung recruitment [6].
HFNC delivers flow, not pressure like CPAP or BiPAP, but the flow can generate an estimated 2-5 cm H2O of PEEP.
HFNC is a better oxygen delivery and respiratory support device than the standard non-rebreather oxygen mask, venturi-mask, and simple low flow nasal cannula in a hypoxic patient. In respiratory distress, a patient’s inspiratory flow and minute ventilation are much higher than the 15 L/min flow of oxygen from a non-rebreather mask. This means with each breath room air is being inhaled along with the supplemental oxygen, ultimately decreasing the total FiO2 being delivered to your patient. HFNC can better match the inspiratory flow and minute ventilation of most patients to deliver a consistent amount of oxygen and less inhaled ambient room air [4,7,8].
HFNC can match your distressed patient’s inspiratory flow, high-flow nasal cannula can deliver near 100% FiO2-more than a NRB can.
Patients are able to tolerate the high flow rates from a HFNC because of heating and humidification. Prior to reaching the patient’s nose, the air can be humidified to 100% and warmed to body temperature. This both improves patient comfort and preserves mucociliary function [8]. It improves secretion management and can reduce re-intubation related to upper airway obstruction [9]. It can also decrease the amount of energy the patient expends heating and humidifying inspired air.
Heat and humidification make the high flow tolerable and probably helps with secretion clearance.
Who should be on HFNC?
HFNC works best for patients with hypoxemic respiratory failure—but not from cardiogenic pulmonary edema and not in the presence of concomitant hypercapnia. The most frequent indication for its use in the ED is pneumonia.
HFNC is an exciting and relatively new modality for respiratory support in adults, and consequently the research is continuously changing and always being updated. The FLORALI trial in 2015 randomized hypoxemic patients with PaO2:FiO2ratios of < 300, mostly from pneumonia, to receive oxygen through a facemask, HFNC or NIPPV. While the primary outcome of patients requiring endotracheal intubation after randomization was no different among the treatment modalities, the group treated with HFNC had a decrease in 90 day mortality [3]. The results of this trial support the use of HFNC over NIPPV and simple oxygen devices in patients with hypoxic respiratory failure, mostly from pneumonia. HFNC is being studied in PEEP responsive processes like acute cardiogenic pulmonary edema because of the small increase in PEEP [10]. However, HFNC is not able to achieve the levels of titratable PEEP that can be delivered by NIPPV (i.e. CPAP). For this reason, NIPPV should be used rather than HFNC for severe, acute cardiogenic pulmonary edema [11]. Although HFNC can wash out the dead space that contains CO2, patients with hypercapnia benefit the most from the ventilatory support that is delivered by NIPPV (i.e. BiPAP). In COPD exacerbations with hypercapnic respiratory failure, NIPPV is a proven therapy to reduce mortality and the need for intubation [12]. There is no current data to demonstrate a benefit of HFNC in hypercapnic patients.
HFNC works best for patients with hypoxic respiratory failure without hypercapnia and not from pulmonary edema. Use HFNC in pneumonia, early ARDS, etc.
Prescribing HFNC in the ED
There are only two variables an emergency physician needs to adjust when using HFNC: flow and FiO2. Start the patient on 30-35 L/min and adjust the flow based on the patient’s level of respiratory distress. For example, if your patient has continued tachypnea or distress after 10-15 minutes of therapy at 30 L/min, increase the flow to 40-45 L/min to provide more support. The general principle is the more distress your patient is in, the more flow is needed. In regards to oxygenation, adjust the FiO2 between 21-100% to obtain desired oxygen saturation.
Don’t set it and forget it; increase the flow to match your patient’s distress.
Reassess the patient frequently, and don’t delay intubation if required. A recent study found no respiratory parameters predictive of the need for intubation; however,if your patient has continued tachypnea, hypoxemia, tachycardia, and increased work of breathing after maximizing the flow and FiO2,the patient needs to be intubated [13]. Beware of the patient on 60 L/min of flow and 100% FiO2 who remains in respiratory distress! This patient is failing despite a tremendous amount of support from the high flow device and will need intubation. Anticipate desaturation during an intubation attempt.
Don’t delay intubation if your patient is failing to improve!
HFNC is effective at pre-oxygenation and apneic oxygenation during an intubation attempt. Leave the HFNC cannula in place throughout induction and laryngoscopy, as the continuous high flow promotes apneic gas exchange. One before and after study suggests fewer desaturations with pre-oxygenation from HFNC as compared to NRB in mild to moderately hypoxic ICU patients, but another study suggested no difference in desaturations when used in those with more severe hypoxemia [14,15]. If the patient is already being treated with a HFNC, our practice is to leave it in place with maximal flow and FiO2during induction and laryngoscopy.
If your patient fails and requires intubation, keep it on for pre-oxygenation and apneic oxygenation.
Similarly, in a patient with a difficult airway who requires an awake fiberoptic intubation, consider initiation of HFNC while preparing to intubate. For an urgent orotracheal intubation with a patient sitting upright, this approach offers pre-oxygenation while the proceduralist readies equipment and applies topical anesthetic to the mouth and glottis. The nasal cannula does not obstruct the proceduralist and offers respiratory support during the awake intubation.
Does your patient with a pneumonia have a known difficult airway from laryngeal cancer? Put them on HFNC while doing an awake fiberoptic orotracheal intubation.
In the patient with a terminal illness who presents emergently with respiratory distress, HFNC can be a helpful adjunct in managing the patient’s symptoms while clarifying further goals of care. It offers the benefit of being able to speak, eat, and is better tolerated than NIPPV. If the patient does not wish to be intubated, HFNC can assist with comfort and work of breathing along with other palliative therapies [16].
Use when clarifying goals of care prior to intubation or as a palliative intervention
Conclusion
The patient in the opening case was transitioned from NRB to HFNC 50 L/min and 80% FiO2. Her tachypnea improved, and she appeared more comfortable. This allowed time for the family to arrive and discuss goals of care with the emergency physician and confirm the DNR status of the patient. She was admitted to the hospital on high-flow nasal cannula.
High-flow nasal cannula should be considered a first-line therapy in all patients with hypoxemic respiratory failure not from cardiogenic pulmonary edema and without concomitant hypercapnia. The high flow rate of HFNC offers many advantages over low flow nasal cannula and NRB that include washout of dead space leading to reduction in the work of breathing, better titration of oxygen, heated and humidified gas to promote secretion clearance, and a low level of positive pressure. This therapy may ultimately decrease mortality in patients with pneumonia as compared to NIPPV and low flow oxygen devices. When initiating therapy, start the patient at 30-35 L/min of flow and titrate the flow rate and FiO2to work of breathing and oxygen saturation. Reach for HFNC on your next shift.
Adapted from originally published article by Skyler Lentz and Matthew Roginski: “A Better Way to Treat Hypoxia: High-Flow Nasal Cannula Is a Good First Option.” Emergency Physicians Monthly. 2018 March; 25(3):10-11.
References / Further Reading:
- Hugo Lenglet et al. “Humidified High Flow Nasal Oxygen During Respiratory Failure in the Emergency Department: Feasibility and Efficacy.” Respir Care 2012;57(11):1873-1878.
- Jens Bräunlich et al. “Effects of Nasal High Flow on Ventilation in Volunteers, COPD and Idiopathic Pulmonary Fibrosis Patients.” Respiration 2013;85:319-325
- Jean-Pierre Frat et al. “High Flow Oxygen through Nasal Cannula in Acute Hypoxemic Respiratory Failure.” The New England Journal of Medicine 2015;372:2185-96.
- E. Rithchie et al. “Evaluation of a humidified nasal high-flow oxygen system, using oxygraphy, capnography and measurement of upper airway pressures.” Anaesth Intensive Care 2011;39:1103-110
- Rachel L Park and Shay P McGuiness. “Pressure Delivered by Nasal High Flow Oxygen During all Phases of the Respiratory Cycle.” Respir Care 2013; 58(10):1621:1624
- Jordi Riera et al. “Effect of High-Flow Nasal Cannula and Body Position on End-Expiratory Lung Volume: A Cohort Study Using Electrical Impedance Tomography.” Respiratory Care April 2013, 58 (4) 589-596
- A. B. Sim et al. “Performance of oxygen delivery devices when the breathing pattern of respiratory failure is simulated.” Anaesthesia 2008;63:938-940.
- Nishimura, Masaji. “High-flow nasal cannula oxygen therapy in adults.” Journal of Intensive Care (2015) 3:15
- Gonzalo Hernández et al. “High-flow nasal cannula support therapy: new insights and improving performance.” Critical Care 2017;21:62
- Onlak Makdee et al. “High-Flow Nasal Cannula versus Conventional Oxygen Therapy in Emergency Department Patients with Cardiogenic Pulmonary Edema: A Randomized Controlled Trial.” Ann Emerg Med. 2017;70:465-472
- Vital FMR, Ladeira MT, Atallah ÁN. “Non-invasive positive pressure ventilation (CPAP or bilevel NIPPV) for cardiogenic pulmonary oedema.” Cochrane Database of Systematic Reviews 2013, Issue 5. Art. No.: CD005351. DOI: 10.1002/14651858.CD005351.pub3
- Osadnik CR, Tee VS, Carson-Chahhoud KV, Picot J, Wedzicha JA, Smith BJ. “Non-invasive ventilation for the management of acute hypercapnic respiratory failure due to exacerbation of chronic obstructive pulmonary disease.” Cochrane Database of Systematic Reviews 2017, Issue 7. Art. No.: CD004104. DOI: 10.1002/14651858.CD004104.pub4.
- Frat JP et al. “Predictors of Intubation in Patients with Acute Hypoxemic Respiratory Failure Treated With a Noninvasive Oxygenation Strategy.” Crit Care Med 2018; 46:208-215
- Romain Miguel-Montanes et al. “Use of High-Flow Nasal Cannula Oxygen Therapy to Prevent Desaturation during Tracheal Intubation of Intensive Care Patients with Mild-to-Moderate Hypoxemia.” Crit Care Med 2015; 43:574–583
- Vourc’h, M., Asfar, P., Volteau, C. et al. “High-flow nasal cannula oxygen during endotracheal intubation in hypoxemic patients: a randomized controlled clinical trial.” Intensive Care Med (2015) 41: 1538. https://doi.org/10.1007/s00134-015-3796-z
- Giulia Spoletini et al. “Heated Humidified High-Flow Nasal Oxygen in Adults: Mechanisms of Action and Clinical Applications.” Chest 2015; 148(1): 253-261.






1 thought on “Looking for a Better Way to Treat Hypoxia in the Emergency Department? Reach for High-Flow Nasal Cannula”
Pingback: Länkar v27 | Internmedicin