Author: Summer Chavez, DO, MPH, MPM (Health Policy Fellow @ Georgetown University/Medstar) // Reviewed by: Alex Koyfman, MD (@EMHighAK) and Brit Long, MD (@long_brit)
Case #1
A 68-year-old male with a history of insulin-dependent diabetes mellitus, benign prostatic hypertrophy (BPH) and hypertension (HTN) presents to the ED with fatigue, subjective fevers for two days, and dysuria. He endorses myalgias and lower back discomfort. He denies any recent surgeries, procedures, or antibiotic use. He had an episode of non-bloody, non-bilious vomiting prior to arrival. The patient reports his blood sugars at home today were 273 and 315. He’s currently complaining of bladder pressure and has not voided in 6 hours. He is tachycardic and febrile.
What should you consider in your differential? What tests should you order? What imaging studies might be helpful?
Case #2
An 82-year old man with a history of BPH, HTN, diabetes, coronary artery disease (CAD), and vertigo presents to the ED with weakness. His wife reports that he had a procedure done a few days ago by his urologist, but isn’t sure of the name. He has been vomiting today and appears dehydrated. The patient has been lying in bed since yesterday but is normally quite active with a walker. They have a big trip planned tomorrow and are wondering if they should cancel. Vital signs include HR 90, BP 105/76, RR 13, Temp: 38.4 C, Sat 98% on RA.
What should you look for on exam? What medications should you order? Does the patient need to be admitted?
What is prostatitis?
According to the National Institutes of Health Classification, prostatitis can be divided into several sub-categories:1,2

For the purposes of this article, we’ll focus on acute bacterial prostatitis.
Prostatitis syndromes are relatively common, especially in the non-elderly population.8 The estimated prevalence for all prostatitis syndromes is 8.2%.9 For patients younger than 50 years old, it’s the most common urologic condition and for those older, the third most common diagnosis.3 In men with at least one prior episode of prostatitis, their cumulative probability of having another episode of prostatitis was as high as 50% in patients 80 years of age and increased with age.10 The exact incidence and prevalence of acute bacterial prostatitis is unknown in the emergency department setting, but its estimated that acute bacterial prostatitis contributes to 4-10% of overall prostatitis cases seen in the community.8,11
One of feared complications of acute bacterial prostatitis is a prostatic abscess, “a localized collection of purulent fluid within the prostate.”12 Although prostate abscesses affect male patients, even infants, the highest incidence of prostatic abscess occurs in men in their 50’s and 60’s.13 The most recent epidemiologic estimates from the 1990’s estimated prostatic abscesses affected 0.2-0.5% of male patients and as much as 2.5% of all prostate disease.13 The incidence of prostatic abscess in men with asymptomatic-HIV and AIDS is 3% and 14% respectively.13 Men undergoing a urologic procedure such as prostate biopsy are another notable group, with approximately 10% of these patients developing prostate abscesses 3,13
How does prostatitis occur?
Although the prostate has natural mechanisms to help prevent infection including immunological (manufacturing antibacterial secretions) or mechanical (ejaculation and voiding to flush the prostatic urethra), insufficient drainage or urinary reflux from the urethra or bladder into the prostate can cause calculi, fibrosis or inflammation.3,8 Seeding can also occur from inoculation after procedures involving the urethra and prostate.3,8,11 Acute bacterial prostatitis is most likely caused by an ascending urinary infection to the intraprostatic ducts.3 The organisms that are implicated in prostatitis may also have higher levels of certain virulence factors than compared to simple cystitis or other genitourinary infections.8
What are risk factors for developing prostatitis?
Other risk factors have been mentioned in the literature: trauma, abstinence and dehydration but high-quality evidence supporting this is lacking.14,15
What organisms cause prostatitis?
Similar to the etiology of other genitourinary infections, gram-negative bacteria are the most common cause.8 E. Coli makes up the overwhelming majority (as high as 88% of acute bacterial prostatitis cases).8 Other Enterobacteriaceae species such as Klebsiella and Proteus make up roughly 10-30% of known cases. Less frequently, Pseudomonas and other Enterococcus are implicated.3,8,15 Some consideration should also be given to other organisms, specifically G+ cocci like Staphylococcus aureus as experts believe the prevalence is increasing.3 Bacteremia from Staphylococcus aureusinfections can acutely infect the prostate. This should also warrant investigation for an occult infection elsewhere, such as endocarditis, the soft-tissue or from a vascular catheter—conditions associated with Staphylococcus aureus bacteremia.3,16,17
Special Populations
Individuals with recent prostate procedures may be more likely to be infected by fluoroquinolone-resistant bacteria and Pseudomonas, probably due to the use of prophylactic antibiotics.3,8,11 Chlamydia trachomatis and Neisseria gonorrhoeae may also be seen in sexually active patients, no matter the patient’s age.3,8,11 Apart from the common bacterial pathogens, patients with HIV may also have Salmonella typhi or Neisseria gonorrhoeae.8,11 Travelers to Asia and Australia may have Burkholderia pseudomallei, which has also been linked to the development of prostatic abscesses.8 Immunocompromised groups, such as patients with diabetes or HIV are more likely to develop prostatic abscesses.8
Clinical Presentation of Acute Bacterial Prostatitis
Classically, patients with acute bacterial prostatitis will present with fever and constitutional symptoms in addition to urinary complaints such as urge incontinence or hesitancy.3,8,11,14 They may also report cloudy urine and genitourinary pain.3,8,11,14 Other patients may merely present with flu-like symptoms (nausea, weakness, chills) so taking a good history is critical to making sure you don’t miss this diagnosis.8,11
Physical Exam
When approaching the physical exam in male patients with genitourinary complaints, providers should be sure to visually inspect the perineum and genitalia, palpate for masses or other abnormalities and perform a digital rectal exam.2,3,11 The prostate is usually tender, edematous and boggy on digital rectal exam, with a sensitivity of 63.3% and specificity of 77.7%.3,11,18 Other sources report more than 95% of patients have prostate tenderness on exam. 13 Fluctuance may be suggestive of an abscess, with a broad incidence of 16-88%.8,13 In some cases, this is all that is needed to establish the diagnosis. Prostate massage is not recommended, but gentle prostate palpation itself is generally safe.2,3 Palpation of the abdomen to investigate bladder distension or flank tenderness can also be helpful when considering other diagnoses.11 Rectal sphincter spasm may also be present.14
Laboratory & Imaging Studies
Although not definitely needed to clinch the diagnosis, patients may have leukocytosis and elevated inflammatory markers such as ESR or CRP.8 No quantitative studies currently exist evaluating their role in diagnosing acute bacterial prostatitis.19 Serum PSA is typically not available in the emergency department and is of limited utility in the acute phase of illness.2,8 Urinalysis may be remarkable for bacteria and pyuria.8 Mid-stream urine culture results along with gram stain are also helpful to determine the responsible microbe.8 (Canadian Urological Association: Level IIA Recommendation).2,8,20 Urine testing before and after prostatic massage has been used to diagnose chronic prostatitis, but prostate massage is contraindicated in in acute bacterial prostatitis due to concern to cause bacteremia.11 One study determined the sensitivity of nitrites was 55-58% and leukocyte esterase was 81-83% in patients with acute bacterial prostatitis.21 Testing for gonorrhea and chlamydia should be considered in sexually active patients.8 Unless patients have valvular disease, concern for endocarditis or sepsis, routine blood cultures are not necessary.8
Bottom Line: Prostatitis is a clinical diagnosis! UA and urine culture may be negative, so be sure to consider the bigger clinical picture.14
Imaging studies are not typically needed unless there is a high suspicion for prostatic abscess or the patient is high risk, with ultrasound and CT being potential imaging modalities (Canadian Urological Association: Level IIIB/IIA Recommendation).2,15 Transrectal ultrasound is recommended first-line as a common and inexpensive imaging modality compared to other imaging alternatives, with a sensitivity of 80-100% for prostatic abscesses.13,22,23,24,25 However, this modality is contraindicated in patients with intense pain, fistulas and severe hemorrhoids.13 This approach also has the benefit of therapeutic intervention such as needle aspiration, with one case series reporting a success rate of 86%.13,23 CT imaging with and without IV contrast can be useful when determining the extent of disease, i.e. concerning for necrotizing spread and is the preferred imaging modality to evaluate for emphysematous prostatic abscesses.13 There are no recent studies evaluating the sensitivity and specificity of CT in diagnosing prostatitis or prostate abscesses.26 Although MRI imaging has a higher sensitivity than CT, it has not been shown to be better than transrectal US.13


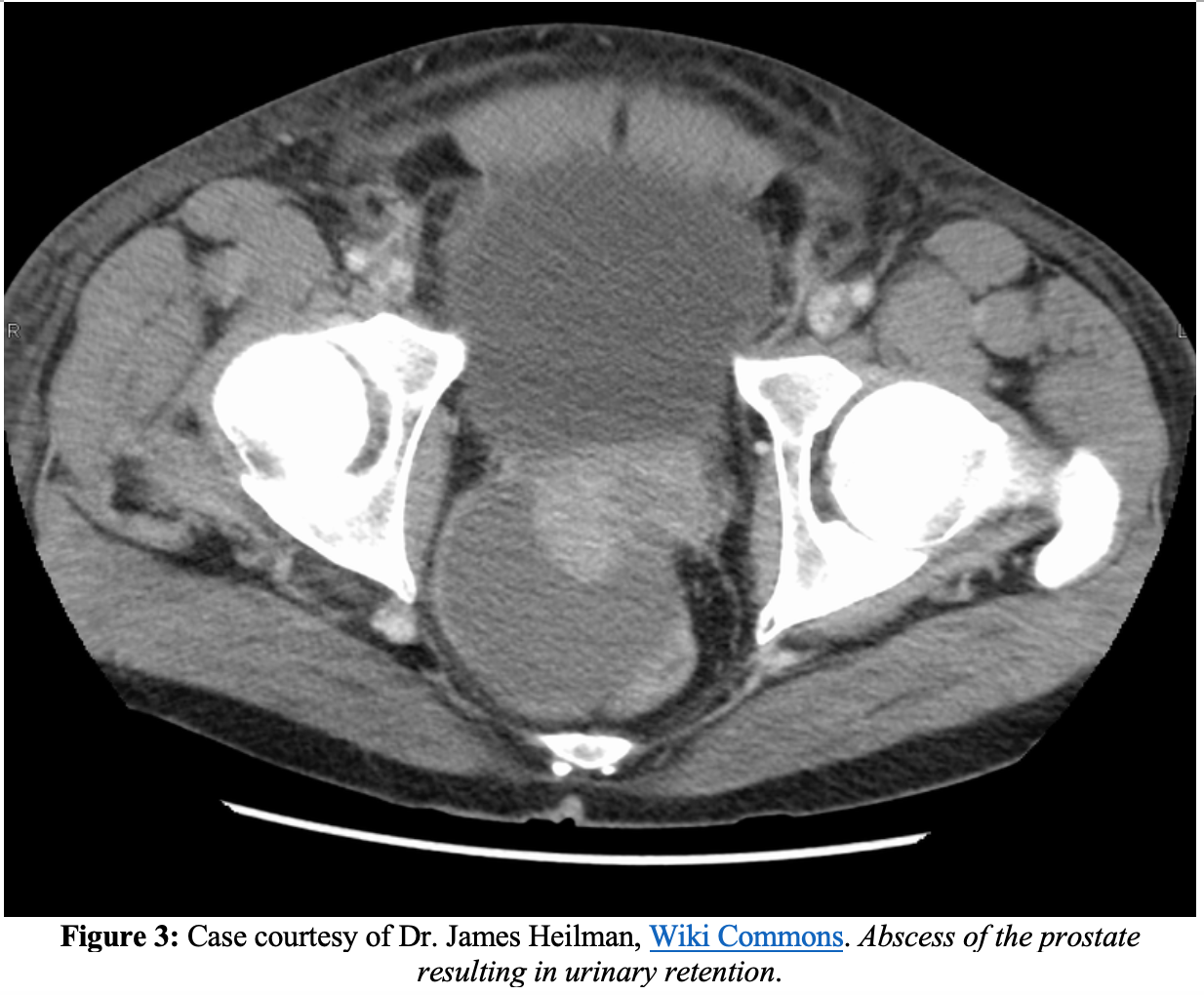
Complications
Aside from endocarditis, epididymitis, further spread of infection into the bone or joint spaces, and development into chronic prostatitis, one of the most serious complications of acute prostatitis is a prostatic abscess. On CT imaging, prostatic abscesses appear as fluid collections that are non-enhancing.13 Prostatic abscesses will appear anechoic or hypoechoic areas on transrectal ultrasound.13 Urology evaluation for possible drainage of the abscess may be required if a prostatic abscess continues after at least a week of antibiotics, in certain refractory patients or those who have failed treatment (Canadian Urological Association: Level IVA Recommendation).2,15
Acute urinary retention is a known complication of acute prostatitis.8 Some sources recommend forgoing typically urethral Foley catheter insertion in lieu of suprapubic catheterization due to potential risk for abscess rupture or septic shock.8 Others recommend either a single catherization with a voiding trial or short-term small-caliber urethral foley catheter.2 Urology consultation is recommended.2,8,14,15
Differential Diagnosis
Perhaps the most significant other alternative diagnosis is a UTI. Recall that either instrumentation through a recent procedure or an anatomical abnormality such as stricture or BPH can predispose individuals to develop UTIs and thus, prostatitis. Patients who do not respond to treatment for acute cystitis should be worked up for potential prostatitis. While patients with BPH may report urinary symptoms, they should not have fever or other infectious findings in their laboratory evaluation. Prostate tenderness can help to differentiate prostatitis from other diagnoses such as epididymitis or urethritis.
Management & Treatment
The mainstay of treatment for uncomplicated acute bacterial prostatitis is antibiotics.
When should patients be admitted?
Patients without findings of hemodynamic instability, concern for impending sepsis, significant comorbidities and tolerating PO can be safely managed as outpatients with outpatient urology follow-up.14 Patients who are not reliable, without good follow-up or with high suspicion for bacteremia should be admitted. Finally, patients who develop acute urinary retention should be closely monitored as they may require bladder catheterization and subsequent hospitalization.2
What’s the best antibiotic to use?
Although no evidence from comparative trials exists, local resistance patterns and antibiograms should be taken into consideration. Trimethoprim-sulfamethoxazole should not be used as a first-line agent if regional E. Coli resistance is more than 10-20%.2 Fluoroquinolones have higher cure rates, but consider the side effect and potential adverse reactions with your patients.14 Make your treatment choice based on the most likely organism, which for most individuals means that gram negative coverage is key.

Consider adding an aminoglycoside if the patient recently took antibiotics or appears septic.3 Tetracyclines and macrolides have been reviewed in the literature, with limited success compared to these other preferred agents.3 Some controversy exists regarding the ideal duration of therapy, with sources ranging from two to six weeks.2,3,8 Clinically, patients should start feeling better with remission of fever and dysuria within the first week of antibiotic treatment.8,13
Other Considerations
Patients that have never used alpha-blockers before and are newly diagnosed with acute bacterial prostatitis may have symptomatic improvement by adding this to their treatment regimen.2,14 Although urology literature argues alpha-blockers can improve patient symptoms for all types of prostatitis, this is based on varying levels of evidence.2 No specific trials related to acute bacterial prostatitis exist and the data is limited.27 Further decisions regarding which alpha blockers and at which doses can be made in conjunction with urology. NSAIDs can also be of some use.2 Other non-pharmacological interventions including repetitive prostatic massage do not strongly support their inclusion.2,3
Case #1
The patient’s physical exam is remarkable for prostate tenderness and suprapubic tenderness to palpation. He has no CVA tenderness, making pyelonephritis less likely. He has no testicular pain, making epididymitis and torsion less likely. He has no murmurs, rubs or gallops on exam, making endocarditis or valvular disease less likely. After ordering a UA with reflex culture, CBC, BMP, you perform a bedside ultrasound that shows >500 mL of urine. After speaking with Urology, a small urethral foley catheter is placed with resolution of the obstruction. Urology recommends admitted the patient to the hospitalist and monitoring for clinical improvement for 24 hours before ordering an ultrasound. The patient is started on Zosyn and Gentamicin and goes upstairs shortly afterwards.
Case #2
On exam, the patient is actively vomiting. He has dry mucus membranes but no generalized abdominal discomfort. He has exquisite tenderness to palpation of the prostate without gross blood or other abnormality. His lungs are clear ,and he has no skin findings suggestive of infection. Due to concern for sepsis, CBC, BMP, lactate, blood cultures, UA with reflex culture and fluids are ordered. The patient is empirically started on Ertapenem and a CT scan is ordered to evaluate for potential prostatic abscess. After resuscitation, the patient condition improves and fortunately, the imaging study shows no fluid collection. Urology is consulted regarding the patient and the patient is admitted to the medicine service.
Key Points
- Prostatitis can be tricky to diagnosis, but complete a focused but thorough history and exam. The key to diagnosis is considering the disease. Tenderness on DRE helps to make the definitive diagnosis of prostatitis.
- Patients with recent instrumentation, immunocompromise, diabetes or anatomic abnormalities are at higher risk for prostatitis.
- Patients with sepsis, poor follow-up, acute urinary retention, or concern for other infections such as endocarditis should be admitted.
- Ultrasound or CT imaging can be used to evaluate for prostatic abscess, which should be considered in patients who do not symptomatically improve with antibiotic treatment.
- E. Coli is the most common cause. Consider covering for G+ organisms in patients with a concern for endocarditis, valvular abnormality or other concurrent infection.
References/Further Reading:
- Krieger JN, Nyberg J Leroy, Nickel JC. NIH Consensus Definition and Classification of Prostatitis. JAMA. 1999;282(3):236-237.
- Nickel JC. Prostatitis. Can Urol Assoc J. 2011;5(5):306-315. doi:10.5489/cuaj.11211
- Lipsky BA, Byren I, Hoey CT. Treatment of Bacterial Prostatitis. Clin Infect Dis. 2010;50(12):1641-1652. doi:10.1086/652861
- Prostatitis: Inflammation of the Prostate | NIDDK. National Institute of Diabetes and Digestive and Kidney Diseases. https://www.niddk.nih.gov/health-information/urologic-diseases/prostate-problems/prostatitis-inflammation-prostate. Accessed January 28, 2020.
- Pontari M. Chronic prostatitis and chronic pelvic pain syndrome. Up To Date. http://www.uptodate.com. Published December 2019.
- Lummus WE, Thompson I. PROSTATITIS. Emergency Medicine Clinics of North America. 2001;19(3):691-707. doi:10.1016/S0733-8627(05)70210-8
- Nickel JC, Alexander RB, Anderson R, et al. Category III Chronic Prostatitis/Chronic Pelvic Pain Syndrome: Insights from The National Institutes of Health Chronic Prostatitis Collaborative Research Network Studies. Curr Urol Rep. 2008;9(4):320-327.
- Meyrier A, Fekete T. Acute Bacterial Prostatitis. UpToDate. http://www.uptodate.com. Published December 2019.
- Krieger J, Lee S, Jeon J, Cheah P, Liong M, Riley D. Epidemiology of prostatitis. International Journal of Antimicrobial Agents. 2008;31(Suppl 1):S85-S90. doi:10.1016/j.ijantimicag.2007.08.028
- Roberts RO, Lieber MM, Rhodes T, Girman CJ, Bostwick DG, Jacobsen SJ. Prevalence of a physician-assigned diagnosis of prostatitis: the Olmsted County Study of Urinary Symptoms and Health Status Among Men. Urology. 1998;51(4):578-584. doi:10.1016/s0090-4295(98)00034-x
- Coker TJ, Dierfeldt DM. Acute Bacterial Prostatitis: Diagnosis and Management. AFP. 2016;93(2):114-120.
- Reddivari AKR, Mehta P. Prostate Abscess. In: StatPearls. Treasure Island (FL): StatPearls Publishing; 2019. http://www.ncbi.nlm.nih.gov/books/NBK551663/. Accessed January 26, 2020.
- Ackerman AL, Parameshwar PS, Anger JT. Diagnosis and treatment of patients with prostatic abscess in the post-antibiotic era. International Journal of Urology. 2018;25(2):103-110. doi:10.1111/iju.13451
- Davis J. Male Genital Problems. In: Tintinalli’s Emergency Medicine: A Comprehensive Study Guide. 8th ed. McGraw-Hill Education; 2016:601-608.
- Davis NG, Silberman M. Bacterial Acute Prostatitis. In: StatPearls. Treasure Island (FL): StatPearls Publishing; 2019. http://www.ncbi.nlm.nih.gov/books/NBK459257/. Accessed January 15, 2020.
- Schattner A, Finn T, Glick Y, Dubin I. Prostate Abscesses and Staphylococcus aureus Bacteremia. The American Journal of Medicine. 2018;131(10):e417-e418. doi:10.1016/j.amjmed.2018.05.031
- Tong SYC, Davis JS, Eichenberger E, Holland TL, Fowler VG. Staphylococcus aureus Infections: Epidemiology, Pathophysiology, Clinical Manifestations, and Management. Clinical Microbiology Reviews. 2015;28(3):603-661. doi:10.1128/CMR.00134-14
- Smithson A, Ramos J, Netto C, Adrián M, Bruno C, Bastida M. Acute prostatitis in men with urinary tract infection and fever: diagnostic yield of rectal examination findings in the emergency department. Emergencias. 2012;24:292.
- Prostatitis – Infectious Disease and Antimicrobial Agents. http://www.antimicrobe.org/e53.asp. Accessed January 28, 2020.
- Sharp VJ, Takacs EB, Powell CR. Prostatitis: Diagnosis and Treatment. AFP. 2010;82(4):397-406.
- Etienne M, Pestel-Caron M, Chavanet P, Caron F. Performance of the Urine Leukocyte Esterase and Nitrite Dipstick Test for the Diagnosis of Acute Prostatitis. Clin Infect Dis. 2008;46(6):951-953. doi:10.1086/528873
- Trauzzi SJ, Kay CJ, Kaufman DG, Lowe FC. Management of prostatic abscess in patients with human immunodeficiency syndrome. Urology. 1994;43(5):629-633. doi:10.1016/0090-4295(94)90176-7
- Lim JW, Ko YT, Lee DH, et al. Treatment of prostatic abscess: value of transrectal ultrasonographically guided needle aspiration. J Ultrasound Med. 2000;19(9):609-617. doi:10.7863/jum.2000.19.9.609
- American Institute of Ultrasound in Medicin, American Urological Association. Ultrasound Examination in the Practice of Urology. https://www.aium.org/resources/guidelines/urology.pdf.
- Barozzi L, Pavlica P, Menchi I, De Matteis M, Canepari M. Prostatic abscess: diagnosis and treatment. American Journal of Roentgenology. 1998;170(3):753-757. doi:10.2214/ajr.170.3.9490969
- Thornhill B, Morehouse H, Coleman P, Hoffman-Tretin J. Prostatic abscess: CT and sonographic findings. American Journal of Roentgenology. 1987;148(5):899-900. doi:10.2214/ajr.148.5.899
- Nickel JC. Alpha-Blockers for the Treatment of Prostatitis-Like Syndromes. Rev Urol. 2006;8(Suppl 4):S26-S34.





