Author: Brit Long, MD (@long_brit, EM Attending Physician, San Antonio, TX) // Edited by: Alex Koyfman, MD (@EMHighAK, EM Attending Physician, UTSW / Parkland Memorial Hospital)
Welcome to EM@3AM, an emDOCs series designed to foster your working knowledge by providing an expedited review of clinical basics. We’ll keep it short, while you keep that EM brain sharp.
A 23-year-old male is brought in by EMS from the scene of a severe accident, in which he was the driver of a motorcycle. He was helmeted. He is hypotensive and tachycardic, with a mangled right lower extremity and right upper extremity. EMS applied a tourniquet to both the right upper and lower extremity. Your initial primary survey reveals properly placed tourniquets. He has bilateral breath sounds. With inward pressure on the iliac wings, you detect pelvic instability.
What’s the diagnosis, and what’s your next step in your evaluation and treatment?
Answer: Apply pelvic binder, concern for open book pelvic fracture
- Anatomy: Pelvis composed of ilium, ischium, pubis, sacrum, coccyx, and ligamental support.
- Pelvic fractures can be broken into acetabular fracture, single bone fracture, pelvic ring fractures.
- Background: Pelvic ring fractures are associated with high energy mechanisms, major hemorrhage that is often difficult to control, and high morbidity and mortality (mortality reaches 50-70% if hemodynamic shock present with open book fracture).
- Mortality in trauma patients is 3X higher with pelvic fracture.
- High risk of associated injuries.
- Open fracture present with open skin or rectal or vaginal involvement.
- Two Classification systems: Tile vs. Young Burgess. Young Burgess is more commonly used in the ED.
- Tile: A (rotationally and vertically stable), B (rotationally unstable, vertically stable), C (rotationally and vertically unstable).
- Young Burgess: anteroposterior compression (APC), lateral compression, vertical shear, combined mechanism.
- APC: often unstable, typically head on MVC for mechanism, often thorax and abdomen injuries, pelvic/retroperitoneal hemorrhage.
- Lateral: most common, typically T-bone MVC or pedestrian hit from side, often stable due to crush inward, may be associated with bladder rupture.
- Vertical shear: mechanism includes vertically oriented force, often unstable with increased pelvic volume.
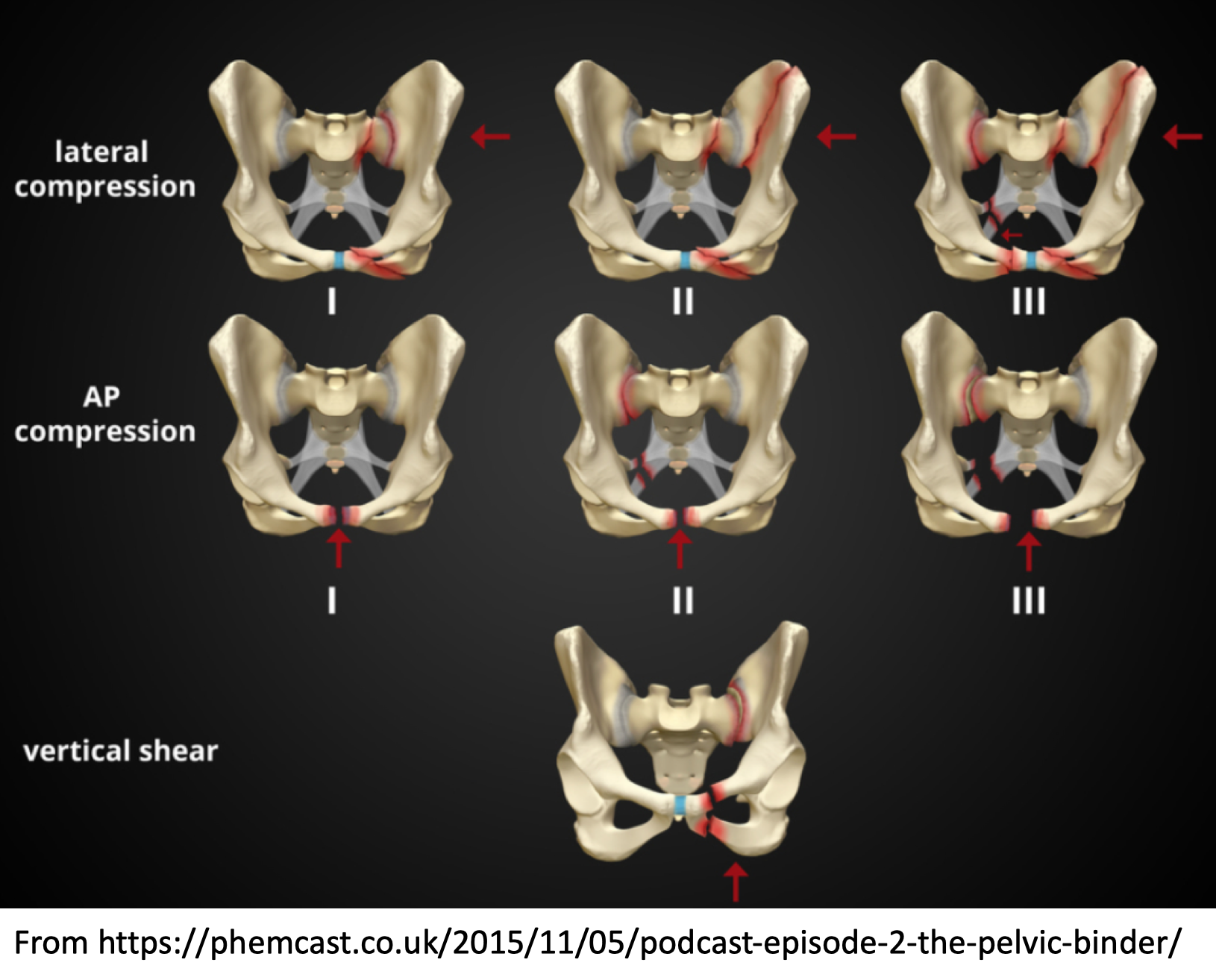
-
- 4 sources of hemorrhage in pelvic fracture: venous (most common, up to 90% of cases), fractured bone surfaces, arterial injury, and extra-pelvic source.
- Arterial source is more common in patients with ongoing bleeding despite pelvic binding.
- True pelvic volume approximates 1.5L, but with disruption of pelvic ring due to fracture, this is greater. The retroperitoneal space can accommodate up to 5L of fluid.
- 4 sources of hemorrhage in pelvic fracture: venous (most common, up to 90% of cases), fractured bone surfaces, arterial injury, and extra-pelvic source.
- History and Exam:
- Evaluation is part of trauma assessment with MARCH approach/Addressing massive hemorrhage then ABCDE.
- History including mechanism of injury, other injuries, initial vital signs, interventions important if available from EMS.
- Pelvis assessment must be performed carefully: Look for deformity, asymmetry, wounds, ecchymoses.
- Assess for pelvic instability/mobility: gentle inward compression of iliac crests performed once; any instability mandates pelvic binder.
- Avoid “rocking” the pelvis or multiple inward compressions, which can worsen bleeding.
- If suspicion for pelvic fracture is present: examine perineum, genitalia, rectum for open injuries, hematomas, or blood; evaluate lower extremities, neurovascular status, length discrepancy, malrotation; evaluate abdomen for other trauma.
- If the patient is alert with no distracting injury and the exam is normal, pelvic fracture is highly unlikely.
- Diagnostics:
- Laboratoy assessment
- VBG can provide information on hemoglobin, pH, lactate, base deficit.
- Beta HCG in females.
- Hemoglobin/hematocrit, renal/liver function, TEG (if available, otherwise coagulation panel).
- Diagnostic peritoneal aspirate (DPA)
- Performed above umbilicus in patients with suspected pelvic fracture.
- Positive if aspiration of 10 mL of blood or GI contents.
- May rule out false negative FAST in unstable patient.
- Imaging
- FAST scan: assess for intraperitoneal fluid.
- Positive scan predicts intraabdominal injury and need for laparotomy; highly specific.
- Negative scan cannot exclude injury, as negative FAST can miss 20-77% of injuries.
- False positives may occur in the setting of bladder rupture.
- AP pelvis x-ray: normal x-ray cannot rule out pelvic fracture; however, it can be used to exclude pelvic fracture as the cause of hemodynamic instability if normal.
- Obtain pelvic x-ray if patient is unstable, altered/confused, has distracting injuries, is pediatric, or if CT of the abdomen/pelvis is not to be completed.
- Do not obtain pelvic x-ray if the patient has a normal exam, is alert with no distracting injuries, and is able to ambulate. Pelvic x-ray may also not be needed if the patient is stable and an abdominal/pelvic CT will be obtained.
- Sensitivity of pelvic x-ray is 64-78% when compared to CT.
- CT of the abdomen/pelvis with IV contrast
- Modality of choice for pelvic ring injury assessment.
- Should be performed in stable patient to evaluate for other injuries and determine severity of fracture.
- Angiography can be used for arterial injury and embolization.
- FAST scan: assess for intraperitoneal fluid.
- Laboratoy assessment
- Complications
- Major hemorrhage/shock, which are the leading cause of death.
- Other injuries:
- Acute: Intraabdominal (28%), hollow viscous (13%), rectal/vaginal (5%), aorta rupture, GU injuries include bladder and urethral injuries (up to 20% of cases), nerve injury to L4-S5, ileus, fat embolization, abdominal compartment syndrome, ARDS, venous thromboembolism.
- Late: Disability, incontinence, sexual dysfunction, infection, complications of fracture.
- Management
- Assess and treat other injuries; provide hemostatic resuscitation (massive transfusion, TXA).
- Stabilize pelvis: avoid patient movement if able, apply pelvic binder early.
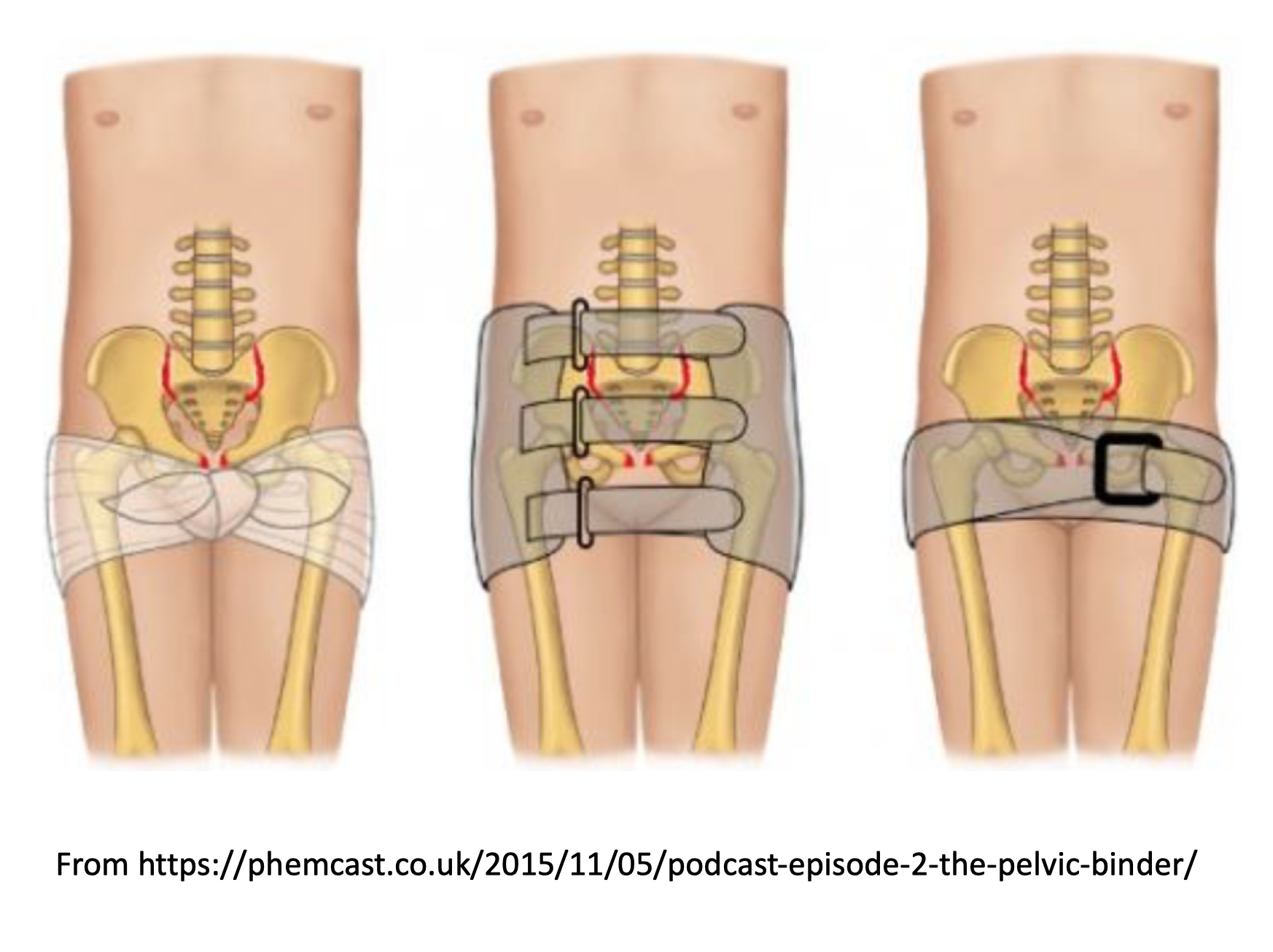
- Discuss patient with trauma surgery and orthopedics early for patients with pelvic fractures.
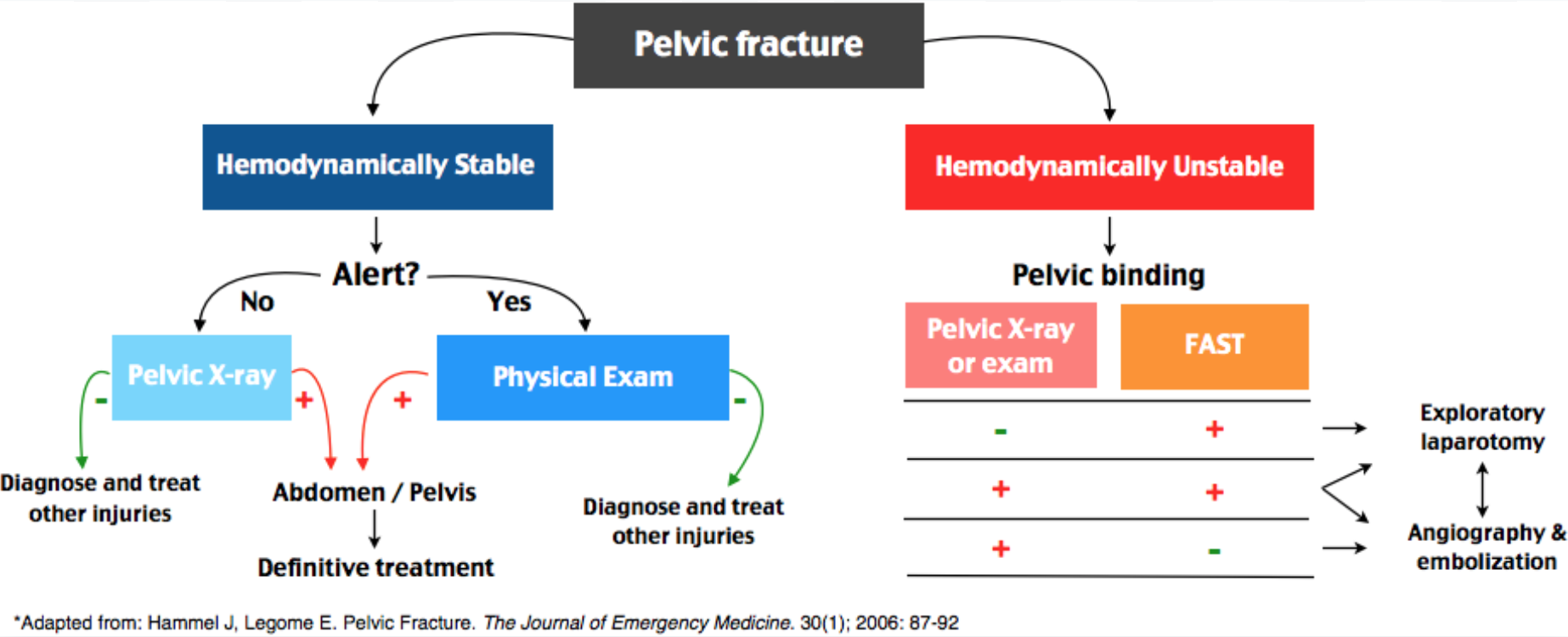
- If stable: Apply binder, perform CT with contrast; if blush present, angiography may be needed.
- If unstable: Hemostatic resuscitation, apply binder, obtain FAST and AP pelvic x-ray.
- Normal pelvic x-ray can exclude pelvic cause of instability.
- FAST negative, then consider REBOA zone III, preperitoneal packing and to OR. DPA may be useful (positive, then go to OR).
- FAST positive, then laparotomy with pelvic stabilization/pre-peritoneal packing. Consider REBOA zone I (if extended time to OR).
- 3 options for unstable patient with pelvic fracture: angiography with embolization (useful for arterial bleeding), packing (decreases venous bleeding), or external fixation and mechanical stabilization.
- REBOA may be required (zone III for pelvic fracture as cause of instability).
- Provide analgesia early in care.

- Disposition
- OR and/or IR if positive FAST with pelvic fracture or positive DPA.
- If REBOA placed, patient requires OR.
- ICU after OR/IR.
- Floor for stable patients with pelvic fracture.

A 35-year-old man presents as a trauma after a T-bone motor vehicle collision to the passenger side. He was a restrained passenger and the airbags deployed. On arrival, he is backboarded and in a cervical collar. Vital signs include blood pressure of 88/62 mm Hg, heart rate of 132 bpm, respiratory rate of 18 bpm, oxygen saturation of 97% on room air, and Glasgow coma scale score of 15. Vascular access is obtained and 2 liters of normal saline are administered, but his vital signs only improve slightly. His extended focused assessment with sonography for trauma scan is negative. His pelvis shifts during assessment for stability. An X-ray of his pelvis is consistent with lateral compression fractures. Following the initiation of a blood transfusion, which of the following is the next best step?
A) Angiographic embolization
B) Computerized tomography scan of the abdomen and pelvis
C) Observation
D) Pelvic binder placement
Answer: A
Pelvic fractures are associated with a high morbidity and mortality. Most pelvic fractures are due to automobile related injuries. However, in the elderly, even minor trauma can result in a fracture. The pelvis is a complex structure functioning in structural, protective, and hematopoietic roles. It is comprised of three bones (ischium, ilium, and pubis) that attach to the sacrum to create a ring. The mechanism of injury is often a determinant of the pattern of injury. In an unstable patient with a pelvic fracture, efforts must be made to evaluate for bleeding into other body cavities. Angiographic embolization of bleeding pelvic vessels in an unstable patient is an effective mechanism for controlling arterial bleeding of the fractured pelvis and should be considered early in hemodynamically unstable patients with pelvic fractures after other sources of bleeding have been excluded.
A computerized tomography scan of the abdomen and pelvis (B) is useful for diagnosing injuries in a stable trauma patient. Unstable patients should not be sent out of the department unless it is for definitive care. This patient will likely need observation (C) in the intensive care unit after he is stabilized, but control of his bleeding must be obtained prior to observation. A pelvic binder (D) is a great option in a patient with an open book pelvic fracture, but in a lateral compression fracture pattern of injury the pelvis is already internally rotated and further lateral compression may worsen injuries.
FOAMed:
Life in the Fast Lane Classification of Pelvic Fractures
References:
- Demetriades D, et al. Pelvic fractures: epidemiology and predictors of associated abdominal injuries and outcomes. J Am Coll Surg. 2002 Jul;195(1):1-10.
- Giannoudis P V., Grotz MRW, Tzioupis C, et al. Prevalence of Pelvic Fractures, Associated Injuries, and Mortality: The United Kingdom Perspective. J Trauma Inj Infect Crit Care. 2007;63(4):875-883.
- Obaid, AK, Barleben A, Porral D, et al. Utility of plain film pelvic radiographs in blunt trauma patients in the emergency department. Am Surg. 2006; 72(10):951-954.
- Davis, J. W., Moore, F. A., McIntyre, R. C., et al. Western Trauma Association Critical Decisions in Trauma: Management of Pelvic Fracture With Hemodynamic Instability. The Journal of Trauma: Injury, Infection, and Critical Care 2008;65(5):1012–1015.
- Cullinane DC, Schiller HJ, Zielinski MD, et al. Eastern Association for the Surgery of Trauma Practice Management Guidelines for Hemorrhage in Pelvic Fracture—Update and Systematic Review. J Trauma Inj Infect Crit Care. 2011;71(6):1850-1868.
- Skitch S, Engels PT. Acute management of the traumatically injured pelvis. Emerg Med Clin N Am. 2018;36:161–179.





