Authors: Mary Hamblen, DO (EM Resident Physician, TX); Justin Hacnik, MD (EM Resident Physician, TX); Katherine Spencer, MD (EM Resident Physician, TX); J.D. Cambron, DO (EM Attending Physician, TX) // Reviewed by: Joshua Lowe, MD (EM Attending Physician, USAF); Marina Boushra, MD (EM-CCM Attending, Cleveland Clinic Foundation); Alex Koyfman, MD (@EMHighAK); Brit Long, MD (@long_brit)
Case
A 37-year-old male presents to the emergency department with a severe, unrelenting headache that started suddenly while lifting weights at the gym 1 hour prior to arrival. The headache is described as diffuse, sharp, and maximal in intensity within a few minutes from onset. He also reports associated photophobia, nausea, and a single episode of vomiting in the lobby. He denies a history of similar headaches in the past.
He denies any medical history, significant family history, or recreational drug use.
Vital signs: Temperature 99.5F, HR 98 bpm, BP 162/86 mmHg, RR 14 per minute, oxygen saturation 99% on room air.
The exam reveals an uncomfortable patient, with difficulty keeping his eyes open. His visual acuity is intact, extraocular movements are intact bilaterally with pupils equal and reactive to light. Examination of the strength and sensation of his extremities reveals no abnormalities, and he is not experiencing scalp tenderness to palpation.
A non-contrast CT study of the brain reveals hyperattenuation at the level of the suprasellar cistern concerning for a spontaneous subarachnoid hemorrhage (SAH). Given the patient’s history and presentation, should a CTA head and neck be obtained to evaluate for aneurysm?
The use of CTA (computed tomography angiography) in the emergency department (ED) has increased dramatically in the past 20 years.1 One study found that CTA head and neck was ordered for 2.5% of all patients in the ED for over 800 different stated indications.2 Outcomes of patients presenting with ischemic stroke who received MRI as initial imaging modality have demonstrated similar outcomes to those with initial CTA, with Kim et al. demonstrating that functional outcome at 3 months did not differ between the CTA and MRI groups (38.5% vs. 38.1%) with a good functional outcome.3 CTA is also more readily available and less invasive than traditional catheter angiography. Similarly, CTA head/neck is more widely available, relatively cheaper, and much faster to obtain than MRI, while still retaining a high level of accuracy.4 Despite it being the cheaper option when it comes to vascular imaging, it is not cheap: national average for CTA head and neck together in the United States of America (without insurance) is around $4500.5, 6 Further, any use of imaging prolongs ED stays, which by extension increases ED wait times for other patients.7
Indications
In general, the use of CTA generates a rapidly obtained map of all major vessels within the brain and neck, which is useful when vascular abnormalities are in the differential. Potential findings include, but are not limited to: arterial aneurysms or dissections, large vessel occlusions, vasculitis and collagen vascular diseases, tumors of vascular origin, vertebrobasilar insufficiency, carotid stenosis, and hemorrhagic metastases. There is a finite amount of pathology detectable by CTA head/neck that is represented by seemingly infinite constellations of symptoms among different patients. In a study of 17,903 CTAs ordered in the ED, Tu et al. (2021) found that the top 5 reasons for ordering a CTA head/neck were suspected stroke, neurologic problem, dizziness, headache with new/concerning symptoms, and altered mental status.2 In total, they found 833 discrete chief complaints used as justification for ordering a CTA head/neck, and these included complaints such as lethargy, back pain, syncope, trauma, hypertension, and arm pain.2 Various clinical guidelines and risk calculators exist to help the ED physician decide whether to use CTA in their evaluation, but they are not comprehensive. This review covers the more common presentations triggering the use of CTA head/neck and whether it is indicated in those settings.
Stroke
Authors’ Recommendation: CTA head/neck should be acquired in patients with stroke symptoms presenting within 24 hours of symptom onset.
One of the most common uses of CTA head and neck is in the evaluation of the patient presenting with acute ischemic stroke (AIS) symptoms, with the primary intention being the potential discovery of a vascular lesion amenable to mechanical thrombectomy (MT).2 CTA head/neck is typically performed in combination with non-contrast CT (NCCT) head as part of most institutional stroke protocols. In the past, CTA was reserved for patients with NIHSS (National Institutes of Health Stroke Scale) ≥ 6, but those guidelines have been challenged.8 The data in Mayer et al. (2019) argue against a minimum NIHSS score to trigger the use of CTA, instead purporting that clinical suspicion of acute ischemic stroke presenting within 24 hours of the last known well was sufficient evidence to order the study. By following this protocol, detection of LVOs (large vessel occlusions) was significantly increased by 7%.8
The VAN (vision, aphasia, neglect) score (Figure 1), first proposed by Teleb et al. in 2016, is a more succinct evaluation for LVO that has been shown to be as sensitive and more specific than the NIHSS.9 A later assessment of the VAN score in Beume et al. noted that it was limited by the stipulation that the patient is “VAN-negative” if they lack motor weakness, halting any subsequent evaluation of cortical symptoms such as aphasia and neglect.10 They instead proposed that cortical symptoms alone or in conjunction with hemiparesis were highly sensitive for LVO, without necessitating a cut-off score or prerequisite exam finding.10 This is addressed in a prior emDOCs article: http://www.emdocs.net/diagnosis-and-neurointerventional-management-of-large-vessel-occlusion-acute-ischemic-stroke/.
Figure 1: Vision, aphasia, neglect emergent large vessel occlusion screening tool.9

There are some who suggest that CTA head and neck should be acquired in patients who are mechanical thrombectomy candidates to help the neuro-interventionalist plan their approach.11 CTA can be helpful for delineating the site and length of the occlusion, the anatomy and condition of the aortic arch and neck vessels, and the presence of collateral circulation.12 However, some have argued that the addition of the CTA neck rarely finds any anatomical variant that significantly prolongs angiography and thus may be less useful except in cases of aneurysm or arteriovenous shunt.13, 14 Regardless of the controversy, the value of MT has been repeatedly shown to improve modified Rankin scores at 90 days, and the use of CTA to justify this intervention is not disputed.15 Even though only a small percentage of CTAs (around 1-3%) reveal intervenable LVOs, the cost over time of missing just one LVO far outweighs the cost of innumerable nondiagnostic CTAs. 2, 16 Each hour of delay to mechanical thrombectomy for LVO is associated with 2-4% increased mortality and 7-10% decrease in good functional outcomes.12
CTA head/neck may be helpful in other respects, such as anticipating prognosis following the use of tissue plasminogen activator (tPA). The presence of residual flow through an occlusion and shorter length of a thrombus (≤15mm) visualized on CTA increases the chances of successful reperfusion via systemic tPA.12 In those patients with obvious intracranial hemorrhage found on NCCT, CTA can help identify the culprit vascular lesion (e.g. aneurysm, arteriovenous malformation) 14% of the time.12, 14 Some studies have reported that a CTA is as sensitive as a digital subtraction angiogram (conventional angiography) in detecting cerebral aneurysms as long as they are read carefully by a neuroradiologist.17-19 Extravasation from the lesion is sometimes visualized as the so-called spot sign, which predicts expansion of the aneurysmal hemorrhage (Figure 2).12, 20
Figure 2: (Left) Initial non-contrast CT of an intraparenchymal hemorrhage; (Middle) CTA showing “spot sign,” (arrow), which indicates active extravasation into intracerebral hemorrhage and predicts expansion; (Right) Repeat non-contrast CT after 24 hours demonstrating expansion of the intraparenchymal hematoma.12

The decision to order CTA head for patients with acute non-traumatic intracerebral hemorrhage depends upon several factors, including age, NCCT appearance, and location of bleeding. In most patients >75 years of age, intraparenchymal hemorrhage (IPH) is secondary to severe hypertension or amyloid angiopathy, and therefore does not warrant CTA to evaluate for a bleeding source unless there is a concomitant subarachnoid hemorrhage (SAH) or intraventricular hemorrhage (IVH).14 However, in patients <75 years old with SAH or IVH, there is a higher probability of finding vascular anomalies on CTA.14 Location of IPH in the basal ganglia, brainstem, or cerebellum is associated with a high negative predictive value for a causative vascular lesion on CTA.14 However, younger age is associated with a higher likelihood of positive findings on CTA regardless of IPH location, as shown in Romero et al. 21 In the scenario of non-traumatic ICH, it is almost never fruitful to acquire a CTA of the neck, since vascular lesions in this region are rare.14
Trauma
Authors’ Recommendation: CTA head/neck is reasonable in any multisystem blunt trauma, but if unsure, using a scoring system such as the Denver or Memphis criteria, though imperfect, may help with the decision. CTA neck should be performed in stable patients without hard signs of vascular or aerodigestive injury after a penetrating neck injury.
Blunt injury to the carotid or vertebral arteries (blunt cerebrovascular injuries, or BCVI, addressed in another emDOCs article: http://www.emdocs.net/blunt-cerebrovascular-injury-ed-presentations-evaluation-and-management/) is found in up to 1% of patients with blunt trauma and 2.7% of patients with blunt multisystem trauma.22, 23 Both types of injury confer high morbidity and mortality.23 Blunt carotid injury is more likely in patients with at least one of the following: Glasgow Coma Scale (GCS) ≤ 6, fracture of petrous bone, presence of diffuse axonal brain injury, and LeFort II/III fractures.23 Blunt vertebral artery injury has been found to be associated with older age, female sex, lower GCS, presence of neck pain, cervical spine fracture, and blunt carotid injury.23 BCVI should be suspected with any high-energy trauma or any fractures of the maxilla or mandible.24 Of all the listed risk factors, cervical spine fracture had some of the strongest associations with BCVI. However, the presence of any combination of the aforementioned or any neurological deficit warrants ordering of CTA head/neck.25
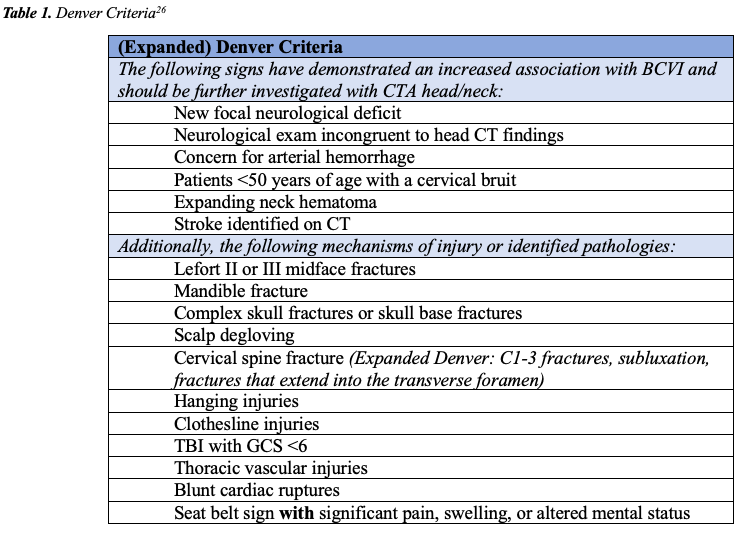
The Eastern Association for the Surgery of Trauma (EAST) recommends using a screening protocol (Denver or Memphis) before ordering a CTA neck for the evaluation of BCVI but does not favor one over the other.26 The Denver Criteria (Table 1) serves as a useful tool to determine which patients are at greater risk for BCVI following blunt trauma to the head or neck.27 Some of the criteria are less useful than others, e.g. isolated seat belt sign without significant pain, swelling, or changes in mental status was shown to have only a 0.5% positivity rate on CTA for BCVI.28 Evaluation of the Denver criteria found that nearly 20% of BCVI, including those with more severe injury, may be missed by the screening tool.29
The Memphis Criteria (Table 2) have been proposed as an alternative to the Denver model in screening for possibility of BCVI and performs approximately as well.30 A later iteration of the Memphis Criteria added basilar skull fracture with involvement of the petrous bone in order to increase the sensitivity of the screening device.31 To date the Denver and Memphis Criteria have not been rigorously compared in the literature and therefore neither has emerged as the superior screening tool. Per EAST guidelines, it is recommended that ED physicians use one of these when making the decision whether to use CTA in blunt trauma. Even with expanded/modified criteria, though, 5% of BCVIs still fall through the screening devices, so EAST recommends using good clinical judgement.26 Indeed, many trauma centers now include CTA head/neck as part of their normal pan-scan for blunt trauma to avoid this issue.32
Table 2: Memphis Criteria.26
With regards to penetrating neck injuries, particularly those in which the platysma is violated, CTA of the neck has allowed a shift away from mandatory operative exploration of Zone 2 neck wounds (those in the mid-neck). The increasingly popular “No Zone” management strategy states that hemodynamically stable patients without “hard signs” (Table 3) of vascular or aerodigestive injury should undergo CTA of the neck. The negative predictive value of this study in the setting of penetrating neck injury is 98-100%.33
Table 3. Hard signs of vascular and aerodigestive injury in penetrating neck trauma.33
Headache
Authors’ Recommendation: CTA head/neck may be obtained in atraumatic headaches that are atypical, acute, and severe, particularly if associated with new neurologic deficits, a known history of intracranial aneurysm, or a history of connective tissue disorders.
Headaches comprise somewhere around 2% of all presenting complaints in ED patients, and around 1% of those are found to have a cerebrovascular cause.34 The patient presenting with an acute severe headache, atypical of their normal headaches, even without neurological deficit, warrants consideration of ordering a CTA head/neck. Studies have shown that up to 7.4% of patients presenting to the ED with an acute severe headache and lack of focal neurologic deficits were the result of significant intracranial pathology, including spontaneous subarachnoid hemorrhage (SAH), unruptured cerebral aneurysm, and cervical dissections, among others- with cerebral aneurysms being the most common.35-37
SAH is one of the most feared causes of acute headaches presenting to the ED. The most common cause of SAH is ruptured intracranial aneurysm, but rates of aneurysmal rupture in patients without a history of subarachnoid hemorrhage or autosomal dominant polycystic kidney disease are fairly low.38 Estimations of unruptured aneurysm in the general population range from 0.2 to 9.9%, depending on the study.38, 39 Overall, the rate of ruptured aneurysms per year is much lower, between 0.05 to 0.5% per year.39 Variations in size factor into the likelihood of rupture: rupture rate for aneurysms smaller than 10mm is 0.5 to 0.7% per year, and rupture rate for larger aneurysms (10mm or more) is around 1% .38, 39 Location at the basilar tip or within the vertebrobasilar or posterior cerebral circulation has also been shown to increase risk of rupture.39
Risk factors associated with SAH include maximal pain intensity at onset, association with exertion or trauma, witnessed loss of consciousness, neck pain or stiffness, limited neck flexion on exam, age >50 years, and use of anticoagulants/antiplatelets.34, 40 SAH can be diagnosed with NCCT, but CTA head can be used to locate the causative aneurysm as well as any other, yet unruptured, aneurysms present.1 A small caveat here is that the American Heart Association (AHA) recommends conventional angiography over CTA for diffuse SAH.40 CTA has a sensitivity of 97% for cerebrovascular pathologies causative of SAH, but it is not recommended as primary diagnostic test to rule out SAH, with sensitivity as low as 61% for SAH in one study.40
If the NCCT is negative but suspicion for SAH is still high, and it has been >6 hours from symptom onset, a lumbar puncture (LP) is recommended.40 CTA should follow if LP is especially bloody (>5 RBCs/mm3) in the context of negative NCCT. If CTA is negative for any cerebrovascular pathology, then patients are considered low risk for future SAH and safe for discharge.
There are some who advocate skipping the LP in this situation and going straight to CTA instead, relying on the rationale that most SAH (85%) are caused by aneurysmal rupture.42 This post discusses the subject in more detail: http://www.emdocs.net/subarachnoid-hemorrhage-why-do-we-miss-it/. American College of Emergency Physicians (ACEP) gave a level C recommendation that either LP or CTA could be used to rule out SAH after a negative NCCT.40 The American Academy of Emergency Medicine (AAEM) released a position statement in 2014 advocating for the use of CTA in place of LP when LP cannot be done or has equivocal results.42 AAEM noted that 64-slice CTA has a sensitivity of 98% and specificity of 100% for aneurysms >3mm, while LP has 100% sensitivity but 65% specificity for SAH, due to the possibility of a traumatic tap obscuring the result.42 To date, there has not been a rigorous study comparing the sensitivity of one method over the other, and because of this, AHA continues to recommend the acquisition of LP, followed by CTA if positive, as part of the workup for suspected SAH with negative NCCT and >6 hours from symptom onset.40
If it has been less than 6 hours from onset of symptoms, and NCCT is negative, AHA leaves further workup to the physician’s discretion (i.e. LP and CTA are not mandated in this context). A negative NCCT and absence of new neurological deficits within 6 hours of symptom onset is likely enough to rule out SAH. This is especially true if high-quality CT scanners are used and the images are read by board-certified neuroradiologists.40
Cerebral aneurysms are not expected to cause headaches unless they are bleeding or causing compressive symptoms.37, 43 Therefore, routine CTA head/neck to evaluate for unruptured aneurysm in patients with headache, without history or family history of cerebral aneurysm, normal LP, and normal NCCT, is not recommended.40
In patients with a known history of small unruptured aneurysms without a history of SAH, AHA recommends repeat evaluations at regular intervals for size/morphology changes with CTA or MRA (magnetic resonance angiography). Follow-up imaging is recommended once per 1-2 years, with the first screen to occur 6-12 months from the initial discovery.43, 44 For tiny (≤ 3mm) aneurysms with no appreciable growth, repeat imaging can be stretched to every 5 years.45 For patients who have a history of SAH secondary to a ruptured aneurysm, there is a higher risk of future rupture from another aneurysm if present.38 Therefore it is reasonable to perform CTA head/neck in such a patient if they are presenting with the classic signs/symptoms of SAH, especially if they have not been following up for their regular screening CTAs.
Cervical (carotid or vertebral) artery dissection is a very uncommon cause of headache that occurs in younger people, often with neck pain and a delayed focal neurological deficit. The deficit is delayed because the dissection itself leads to thrombosis and then embolization of the thrombus into the cerebral circulation. Patients may present with partial Horner’s syndrome (miosis + ptosis). The headache itself is often sudden onset and limited to the side of the affected vessel. CTA head/neck is absolutely indicated if suspicion is high for this condition.34 Risk factors are the same as those for other vascular causes of headache: connective tissue diseases, such as systemic lupus erythematosus, Behcet’s disease, sarcoidosis, and/or vasculitis.34
Altered Mental Status
Authors’ Recommendation: CTA head/neck is not indicated for altered mental status that is otherwise not associated with acute stroke, severe trauma, or other focal neurologic deficits
Altered mental status encompasses a wide range of disorders including confusion, delirium, lethargy, delirium, psychosis, inappropriate behavior, unresponsiveness, and coma.46 All of these states are some gradation of consciousness impairment.47 Commonly, the cause of a patient’s altered mentation is secondary to: intoxication, organ dysfunction, metabolic or endocrine dysfunction, and even neurologic causes such as traumatic brain injury, seizures, CNS infection including abscess, encephalitis, meningitis, masses, hydrocephalus, PRES (posterior reversible encephalopathy syndrome), and various inflammatory disorders. Often multifactorial, most of the causes can be appropriately diagnosed without the use of CTA. Even NCCT, often performed in these patients, has been found to be low yield in patients with acute atraumatic altered mental status.48
This is not to say that CTA head/neck should never be ordered on patients with altered mental status, only that it should be done so judiciously. In the Tu et. al study looking at 700,000 unique ED visits, 117 CTAs were ordered for “unresponsiveness,” and 544 were ordered for “altered mental status.”2 Of those CTAs, 67.5% and 36.2%, respectively, were found to have “findings requiring immediate or urgent intervention.”2 What these data suggest is that the relatively low number of CTAs ordered was probably indicated by unique details of each case and were not done as part of some standard protocol unless another pathology was suspected.
Clinical judgment should guide the decision whether to order CTA or not and should be used in the context of an appropriate history, exam, and lab workup. The bottom line is that CTA is reasonable when some cerebrovascular cause of altered mental status is suggested by the presentation, but it is unlikely to be high-yield in cases of pure, nonfocal, atraumatic altered mentation.
Syncope / Presyncope
Authors’ Recommendation: CTA head/neck is not indicated for syncope without clear focal neurological deficits.
Neuroimaging is not indicated unless the patient’s history and physical exam suggest neurogenic syncope. These include prolonged loss of consciousness, focal neurologic deficits, headache, and/or carotid bruit.49 The American Academy of Neurology recommends, as part of their Top Five Choosing Wisely Recommendations, to not perform imaging of the carotid arteries for simple syncope without other neurologic symptoms.50
Compression syndromes of the vertebral artery at the craniocervical junction are a rare cause of syncope that occurs when the patient turns their head, dubbed “bow hunter’s syndrome”.51 Similarly, Eagle syndrome is a rare cause of recurrent syncope caused by internal carotid artery compression with movement of the head due to an elongated styloid process and/or ossified stylohyoid ligament.52 If either of these rare conditions is suspected based on inciting factors of syncope, then CTA would be the initial imaging modality of choice to identify surrounding anatomical abnormalities. Transcranial doppler or conventional angiogram is required to confirm the diagnosis.53
Dizziness / Vertigo
Authors’ Recommendation: CTA head/neck may be considered in patients with a new presentation of central vertigo, especially if the patient has multiple vascular risk factors (ABCD2 score is >4). CTA head/neck should be obtained in a young adult with new onset central vertigo and a history of recent minor trauma or connective tissue disorder, to rule out vertebral artery dissection.
Dizziness accounts for ~3-4% of all ED visits. Of those, only 1-5% have an infarct.54 Before ordering a CTA head/neck for the dizzy patient, it is important to understand the pathologies for which these studies are evaluating – a posterior stroke or vertebrobasilar ischemia. Vertigo/dizziness is often the primary complaint in a patient presenting with posterior circulation stroke, and it may be rather nebulous.53 Dizziness (47%) is the most frequent presenting symptom of posterior circulation stroke.55 However, evaluation of 407 patients from the New England Medical Center Posterior Circulation Stroke Registry (NEMC-PCR) reveals that other findings are quite common: unilateral limb weakness (41%), dysarthria (31%), headache (28%) and nausea or vomiting (27%). The most frequent signs were unilateral limb weakness (38%), gait ataxia (31%), unilateral limb ataxia (30%), dysarthria (28%) and nystagmus (24%).55, 56
CTA head/neck in patients with a sole complaint of dizziness has been shown to have low diagnostic yield in multiple studies.2 A study by Fakran et al. demonstrated that of 228 patients presenting with isolated dizziness, only 5 had pathologic findings and only 3 of the 228 patients required intervention.57 Indeed, the recent GRACE-3 guidelines do not support routine use of CTA in acute vestibular syndrome (AVS), (acute, continuous dizziness for > 24 hours) unless there is true concern for intervenable large vessel pathology such as positive VAN (see Figure 1).58 They endorse its use for the patients with AVS when there are signs of central vertigo and there is an absolute contraindication to MRI.58 Some also suggest using CTA head/neck for patients with spontaneous episodic vestibular syndrome (s-EVS) when the history is atypical of peripheral vertigo or the ABCD2 score is >3.54
In the context of dizziness, it has been suggested that an ABCD2 score of >3 increases the likelihood of posterior stroke.53 The ABCD2 score is one of the more commonly referred to algorithms for assessing future risk of stroke in patients who present with TIA (transient ischemic attack), with others being the ABCD3, SPI-II. The ABCD2 score is comprised of Age (≥ 60 years), Blood pressure (≥140/90), Clinical Symptoms (weakness, speech impairment), Duration (of symptoms), and Diabetes.59 It assigns a risk score from 0-7, where ≥ 4 is associated with a 3-fold increase in stroke risk within 7 days.59
Interestingly, vertebral artery dissection occurs in patients without typical vascular risk factors such as older age, hypertension, tobacco use, or hyperlipidemia. Therefore, a low ABCD2 score would not be useful in ruling it out.58 Vertebral artery dissection is most commonly found in adults aged 18-45 years who present with dizziness, neck pain, headache, and nausea/vomiting. These patients may have a history of minor trauma (turning their head too quickly, such as at the chiropractor) or connective tissue disorders. CTA head/neck is the study of choice to evaluate for a vertebral artery dissection (Figure 3).
Figure 3: Some common indications for ordering CTA head and neck.

Complications / Considerations / Potential Pitfalls
Hypersensitivity reactions
Most contrast media hypersensitivity reactions are allergic-like reactions, which entail the release of histamine and other mediators from basophils and eosinophils without the mediation of IgE. IgE-mediated reactions to contrast do exist, but they are very rare. However, IgE-mediated or not, anaphylactic shock is possible in either case.60 Patients with a history of atopic conditions such as asthma, those on chronic beta-blocker therapy, and younger females may be at higher risk for these reactions.
The American College of Radiology (ACR) recommends a premedication schedule 12 hours before a contrasted CT with steroids and diphenhydramine in patients who are at high risk for hypersensitivity reaction but recognizes that this is not feasible in the acute setting. For ED patients requiring emergent imaging, they recommend a 4–5-hour steroid/diphenhydramine premedication schedule prior to the contrast load, citing that any shorter premedication phase has not been shown to be effective in preventing hypersensitivity reactions to contrast.60 Clearly this is still unfeasible when a CTA is being ordered prior to patient arrival and done as soon as a patient is rolled into the door of the ED. No acceptable alternative has been offered to the ACR premedication schedule, and evidence for any acute premedication is sparse at best.61 ACEP and the American Academy of Emergency Medicine AAEM do not currently have any recommendations. If the patient is stable enough to wait, the 5-hour pre-treatment is feasible. If not, a risk/benefit discussion should be had with the patient, their family, the radiologist, and the neurologist on the best course of action.
Radiation Exposure
A CTA head/neck delivers about 1-3 mSV of radiation, and coupled with CT head without contrast, the total delivered is 7-9 mSV.12 Lifetime risk of cancer death from the combined stroke protocol (CT without contrast and CTA head/neck) increases by around 0.02-0.04%.12 There is some disagreement in the literature about cumulative radiation dose and risk of cancer, but some studies note increased (3x) risk with cumulative doses of 50 – 60 mSv.37 Some experts recommend that, if the situation allows, MRA be considered instead of CTA to minimize radiation exposure.62 However, the lifetime risk of cancer from a single CTA head/neck is negligible compared to the risk of missing a life-threatening vascular lesion.37
Contrast-Induced Nephrotoxicity (CIN)
This has been a hot-button topic for some time now and bears discussion. The 2020 Consensus Statements from the American College of Radiology (ACR) and National Kidney Foundation (NKF) acknowledge that there is an insufficient volume of controlled studies to differentiate between contrast-induced acute kidney injury (CI-AKI) and contrast-associated acute kidney injury (CA-AKI).63 This is because their definition of CI-AKI is an AKI that ensues within 48 hours of receiving IV contrast in the absence of any “other nephrotoxic factors.” 63 Since the definition of “other nephrotoxic factors” could be broad and difficult to control for in what has mostly been observational studies, this is a problematic diagnosis. CA-AKI, conversely, is defined as any AKI that occurs within 48 hours of receiving IV contrast – it implies correlation only.63
The Bartels et al. paper from 1954 was the progenitor of the concept of contrast nephropathy with its description of a 69-year-old male with multiple myeloma who developed AKI from an intravenous pyelogram. The writers mentioned other similar patients who developed oliguria/anuria following the same procedure and they theorized that the contrast (50% Diodane, a high-osmolar contrast medium) itself was the cause of the AKI.64 Other reports that followed described CA-AKI after receipt of intra-arterial high-osmolality contrast media (HOCM). Given that this contrast was given intra-arterially, it should not be thought of in the same light as intravenous contrast. Many of these studies were observational retrospective reviews without control groups and no consideration of alternative causes for the AKI.65 Additionally, HOCM is not used in present day and has been replaced with low osmolality contrast media (LOCM) and iso-osmolar contrast media (IOCM), which have better side effect profiles and equivalent image quality to HOCM.66 LOCM and IOCM have no difference in risk for AKI in comparison studies.67, 68
More recently, large meta-analyses of controlled studies (including ~20-25,000 patients) done by McDonald showed that rates of AKI were actually lower in patients who received contrasted CT versus those who got NCCT. 69, 70 They also noted no increased need for emergent dialysis or 30-day mortality in patients who underwent contrasted CT compared to those who received CT without contrast, even in patients with preexisting kidney disease.69, 71 Hinson et al. showed no significant elevation in AKI incidence in 1,464 septic patients following contrasted CT versus 1,731 similar patients who got CT without contrast.73 There are a number of similar examples, but the message here is the same: there is no good evidence supporting clinically significant adverse renal outcomes from using modern contrast media for a CT.
The ACR and NKF recommend the use of a contrasted CT regardless of CI-AKI risk alone if it is required to diagnose a life-threatening. 12, 63 Even if contrast-induced nephropathy were a real problem (which evidence does not support), it should not discourage physicians from getting a clinically indicated study that could alter the course of a patient’s outcome. If the CT with contrast is warranted by the clinical scenario, there should be no hesitation in its acquisition.
Thyrotoxicosis
A patient with a history of hyperthyroidism has a (very) low risk of developing thyrotoxicosis secondary to iodinated contrast exposure if they are in their normal state of health. However, if they are already experiencing thyrotoxicosis, contrast should be completely avoided, as it can precipitate thyroid storm.60 Interestingly, there have not been any studies into the efficacy of prophylactic methimazole or propylthiouracil in the prevention of thyroid storm for those at high risk requiring a contrasted CT.
Site of Injection
For all CTAs head/neck, it is best to inject from the right arm to prevent contrast delay in the left brachiocephalic vein and superior vena cava.17 CTA requires a large contrast dose given at a higher speed than a conventional CT with contrast, so any small obstruction has the potential to cause reflux and therefore artifact.74 The left brachiocephalic vein has a much more tortuous path than the right and is more prone to external compression from surrounding structures.74, 75 In addition, the left brachiocephalic vein has a smaller diameter and longer axial length than the right one.74 If limited by a more peripheral injection site such as the forearm, wrist, or hand, a decrease in the flow rate to 1.5ml/sec or less is required.60
Contrast Extravasation
Contrast extravasation can happen with any contrasted CT, but CTAs have an increased risk of extravasation as they require a high-speed bolus of contrast. Most of these injuries are very minor and should be treated with warm or cold compress and elevation of the extremity. Rarely (<1%), severe injury, as manifested by severe pain, swelling, ulcerations, and paresthesias, requires surgical consultation.60
Patient Flow Concerns
The extent of the impact a CTA head/neck has on patient flow through the department depends on the characteristics of an individual facility. In EDs where leadership has not taken care to recognize its potential for creating a bottleneck effect, the CTA can cause substantial delays. CTA head/neck should not be ordered without at least a short evaluation of the clinical scenario and patient history. Various protocols exist to help decrease time spent preparing a patient for a contrast CT scan (see Emory’s CT Passport) once the determination has been made that it is required.7
Poor Image Quality
Several technical errors outside the control of the ER doctor may occur in the acquisition of the CTA head/neck. Even though we cannot do much about them, it is helpful to be aware that they exist. Beam hardening artifacts may be encountered when a large bolus of IV contrast gets concentrated in calcified vessels, often the subclavian, obscuring proper views of the aortic arch.4 The cavernous ICA has an associated venous plexus that may become indistinguishable from the ICA itself if the contrast is poorly timed.1
Case Conclusions
CT Angiogram of the head was obtained which further demonstrated a subarachnoid hemorrhage in the substellar cistern with an associated posterior communicating artery aneurysm. This patient was admitted to the neurological intensive care unit for neurological checks, blood pressure control, and neurosurgical evaluation. They went for formal angiography, which confirmed the aneurysm that was treated with surgical clipping.
Pearls and Pitfalls
- CT Angiography has become a more readily available tool for diagnosis in the emergency department though requires an understanding of its specific uses and indications.
- Acute stroke and trauma remain strong indications for ordering CTAs of the head and neck.
- The utility of CTA head and neck for evaluation of altered mental status, dizziness, and syncope is controversial and may not provide diagnostic utility outside of certain clinical circumstances.
- An understanding of the risks involved including allergic reaction, radiation exposure, contrast extravasation, and contrast-associated nephropathy allows for a thorough risk-benefit analysis prior to ordering these studies.
References
(1) Barkovich, E. J.; Batheja, V.; Hong, T.; Rao, J.; Javan, R. Pearls and pitfalls in emergency CT neuroangiography through the lens of bias and error. Emerg Radiol 2023. DOI: 10.1007/s10140-023-02143-8 From NLM.
(2) Tu, L. H.; Malhotra, A.; Venkatesh, A. K.; Taylor, R. A.; Sheth, K. N.; Forman, H. P.; Yaesoubi, R. Head and Neck CTA Utilization: Analysis of Ordering Frequency and Nonroutine Results Communication, With Focus on the 50 Most Common Emergency Department Clinical Presentations. American Journal of Roentgenology 2022, 218 (3), 544-551. DOI: 10.2214/ajr.21.26543.
(3) Kim, J. T.; Cho, B. H.; Choi, K. H.; Park, M. S.; Kim, B. J.; Park, J. M.; Kang, K.; Lee, S. J.; Kim, J. G.; Cha, J. K.; et al. Magnetic Resonance Imaging Versus Computed Tomography Angiography Based Selection for Endovascular Therapy in Patients With Acute Ischemic Stroke. Stroke 2019, 50 (2), 365-372. DOI: 10.1161/strokeaha.118.023173 From NLM.
(4) Madhuripan, N.; Atar, O. D.; Zheng, R.; Tenenbaum, M. Computed Tomography Angiography in Head and Neck Emergencies. Semin Ultrasound CT MR 2017, 38 (4), 345-356. DOI: 10.1053/j.sult.2017.02.003 From NLM.
(5) New Choice Health, I. CT Angiography – Neck Cost and Procedure Information. New Choice Health: Vol. 2023.
(6) New Choice Health, I. National CT Angiography – Head Procedure Pricing Summary. 2023; Vol. 2023.
(7) Rachh, P.; Pendley, A. M.; Duong, P.-A. T.; Hanna, T. N.; Heilbrun, M. E. Decreasing CT Acquisition Time in the Emergency Department through Lean Management Principles. RadioGraphics 2021, 41 (3), E81-E89. DOI: 10.1148/rg.2021200107.
(8) Mayer, S. A.; Viarasilpa, T.; Panyavachiraporn, N.; Brady, M.; Scozzari, D.; Van Harn, M.; Miller, D.; Katramados, A.; Hefzy, H.; Malik, S.; et al. CTA-for-All: Impact of Emergency Computed Tomographic Angiography for All Patients With Stroke Presenting Within 24 Hours of Onset. Stroke 2020, 51 (1), 331-334. DOI: 10.1161/strokeaha.119.027356 From NLM.
(9) Teleb, M. S.; Ver Hage, A.; Carter, J.; Jayaraman, M. V.; McTaggart, R. A. Stroke vision, aphasia, neglect (VAN) assessment-a novel emergent large vessel occlusion screening tool: pilot study and comparison with current clinical severity indices. J Neurointerv Surg 2017, 9 (2), 122-126. DOI: 10.1136/neurintsurg-2015-012131 From NLM.
(10) Beume, L. A.; Hieber, M.; Kaller, C. P.; Nitschke, K.; Bardutzky, J.; Urbach, H.; Weiller, C.; Rijntjes, M. Large Vessel Occlusion in Acute Stroke. Stroke 2018, 49 (10), 2323-2329. DOI: 10.1161/strokeaha.118.022253 From NLM.
(11) Powers, W. J.; Rabinstein, A. A.; Ackerson, T.; Adeoye, O. M.; Bambakidis, N. C.; Becker, K.; Biller, J.; Brown, M.; Demaerschalk, B. M.; Hoh, B.; et al. 2018 Guidelines for the Early Management of Patients With Acute Ischemic Stroke: A Guideline for Healthcare Professionals From the American Heart Association/American Stroke Association. Stroke 2018, 49 (3), e46-e99. DOI: doi:10.1161/STR.0000000000000158.
(12) Demchuk, A. M.; Menon, B. K.; Goyal, M. Comparing Vessel Imaging. Stroke 2016, 47 (1), 273-281. DOI: doi:10.1161/STROKEAHA.115.009171.
(13) Mehan, W. A.; Stapleton, C. J.; Raymond, S. B. Does including neck CTA in work-up of suspected intracranial hemorrhage add value? Emerg Radiol 2019, 26 (2), 139-143. DOI: 10.1007/s10140-018-1654-3 From NLM.
(14) Camargo, A.; Zacharia, T.; Kanekar, S.; Bruno, M.; Tian, Z.; Zhou, S.; Yousem, D. M. Value of CTA/MRA in the setting of intraparenchymal hemorrhage in the emergency department. Neuroradiology 2023, 65 (1), 97-103. DOI: 10.1007/s00234-022-03080-y From NLM.
(15) Hollist, M.; Morgan, L.; Cabatbat, R.; Au, K.; Kirmani, M. F.; Kirmani, B. F. Acute Stroke Management: Overview and Recent Updates. Aging Dis 2021, 12 (4), 1000-1009. DOI: 10.14336/ad.2021.0311 From NLM.
(16) Salehi, L.; Jaskolka, J.; Ossip, M.; Phalpher, P.; Valani, R.; Mercuri, M. Utilization of CT angiography of the head and neck in the era of endovascular therapy for acute ischemic stroke: a retrospective study. Emerg Radiol 2022, 29 (2), 291-298. DOI: 10.1007/s10140-021-02001-5 From NLM.
(17) Takhtani, D. CT neuroangiography: a glance at the common pitfalls and their prevention. AJR Am J Roentgenol 2005, 185 (3), 772-783. DOI: 10.2214/ajr.185.3.01850772 From NLM.
(18) Altenbernd, J. C.; Fischer, S.; Scharbrodt, W.; Schimrigk, S.; Eyding, J.; Nordmeyer, H.; Wohlert, C.; Dörner, N.; Li, Y.; Wrede, K.; et al. CT and DSA for evaluation of spontaneous intracerebral lobar bleedings. Front Neurol 2022, 13, 956888. DOI: 10.3389/fneur.2022.956888 From NLM.
(19) van Asch, C. J.; Velthuis, B. K.; Rinkel, G. J.; Algra, A.; de Kort, G. A.; Witkamp, T. D.; de Ridder, J. C.; van Nieuwenhuizen, K. M.; de Leeuw, F. E.; Schonewille, W. J.; et al. Diagnostic yield and accuracy of CT angiography, MR angiography, and digital subtraction angiography for detection of macrovascular causes of intracerebral haemorrhage: prospective, multicentre cohort study. Bmj 2015, 351, h5762. DOI: 10.1136/bmj.h5762 From NLM.
(20) Demchuk, A. M.; Dowlatshahi, D.; Rodriguez-Luna, D.; Molina, C. A.; Blas, Y. S.; Dzialowski, I.; Kobayashi, A.; Boulanger, J. M.; Lum, C.; Gubitz, G.; et al. Prediction of haematoma growth and outcome in patients with intracerebral haemorrhage using the CT-angiography spot sign (PREDICT): a prospective observational study. Lancet Neurol 2012, 11 (4), 307-314. DOI: 10.1016/s1474-4422(12)70038-8 From NLM.
(21) Romero, J. M.; Artunduaga, M.; Forero, N. P.; Delgado, J.; Sarfaraz, K.; Goldstein, J. N.; Gonzalez, R. G.; Schaefer, P. W. Accuracy of CT angiography for the diagnosis of vascular abnormalities causing intraparenchymal hemorrhage in young patients. Emerg Radiol 2009, 16 (3), 195-201. DOI: 10.1007/s10140-008-0785-3 From NLM.
(22) Naraghi, L.; Larentzakis, A.; Chang, Y.; Duhaime, A.-C.; Kaafarani, H.; Yeh, D. D.; King, D. R.; de Moya, M. A.; Velmahos, G. C. Is CT Angiography of the Head Useful in the Management of Traumatic Brain Injury? Journal of the American College of Surgeons 2015, 220 (6), 1027-1031. DOI: 10.1016/j.jamcollsurg.2015.03.002.
(23) Drain, J. P.; Weinberg, D. S.; Ramey, J. S.; Moore, T. A.; Vallier, H. A. Indications for CT-Angiography of the Vertebral Arteries After Trauma. Spine (Phila Pa 1976) 2018, 43 (9), E520-e524. DOI: 10.1097/brs.0000000000002420 From NLM.
(24) Kelts, G.; Maturo, S.; Couch, M. E.; Schmalbach, C. E. Blunt cerebrovascular injury following craniomaxillofacial fractures: A systematic review. Laryngoscope 2017, 127 (1), 79-86. DOI: 10.1002/lary.26186 From NLM.
(25) Ho, A. L.; Deb, S.; Kim, L. H.; Haldipur, A.; Lin, S.; Patel, M.; Singh, H. Predictors of Cervical Vertebral and Carotid Artery Dissection During Blunt Trauma: Experience From a Level 1 Trauma Center. World Neurosurg 2020, 137, e315-e320. DOI: 10.1016/j.wneu.2020.01.191 From NLM.
(26) Kim, D. Y.; Biffl, W.; Bokhari, F.; Brakenridge, S.; Chao, E.; Claridge, J. A.; Fraser, D.; Jawa, R.; Kasotakis, G.; Kerwin, A.; et al. Evaluation and management of blunt cerebrovascular injury: A practice management guideline from the Eastern Association for the Surgery of Trauma. J Trauma Acute Care Surg 2020, 88 (6), 875-887. DOI: 10.1097/ta.0000000000002668 From NLM.
(27) Burlew, C. C.; Biffl, W. L.; Moore, E. E.; Barnett, C. C.; Johnson, J. L.; Bensard, D. D. Blunt cerebrovascular injuries: redefining screening criteria in the era of noninvasive diagnosis. J Trauma Acute Care Surg 2012, 72 (2), 330-335; discussion 336-337, quiz 539. DOI: 10.1097/TA.0b013e31823de8a0 From NLM.
(28) Sherbaf, F. G.; Chen, B.; Pomeranz, T.; Shahriari, M.; Adin, M. E.; Mirbagheri, S.; Beheshtian, E.; Jalilianhasanpour, R.; Pakpoor, J.; Lazor, J. W.; et al. Value of Emergent Neurovascular Imaging for “Seat Belt Injury”: A Multi-institutional Study. AJNR Am J Neuroradiol 2021, 42 (4), 743-748. DOI: 10.3174/ajnr.A6992 From NLM.
(29) Leichtle, S. W.; Banerjee, D.; Schrader, R.; Torres, B.; Jayaraman, S.; Rodas, E.; Broering, B.; Aboutanos, M. B. Blunt cerebrovascular injury: The case for universal screening. J Trauma Acute Care Surg 2020, 89 (5), 880-886. DOI: 10.1097/ta.0000000000002824 From NLM.
(30) Miller, P. R.; Fabian, T. C.; Croce, M. A.; Cagiannos, C.; Williams, J. S.; Vang, M.; Qaisi, W. G.; Felker, R. E.; Timmons, S. D. Prospective screening for blunt cerebrovascular injuries: analysis of diagnostic modalities and outcomes. Ann Surg 2002, 236 (3), 386-393; discussion 393-385. DOI: 10.1097/01.Sla.0000027174.01008.A0 From NLM.
(31) Ciapetti, M.; Circelli, A.; Zagli, G.; Migliaccio, M. L.; Spina, R.; Alessi, A.; Acquafresca, M.; Bartolini, M.; Peris, A. Diagnosis of carotid arterial injury in major trauma using a modification of Memphis criteria. Scand J Trauma Resusc Emerg Med 2010, 18, 61. DOI: 10.1186/1757-7241-18-61 From NLM.
(32) Müther, M.; Sporns, P. B.; Hanning, U.; Düsing, H.; Hartensuer, R.; Raschke, M.; Schwake, M.; Stummer, W.; Glasgow, S. Diagnostic accuracy of different clinical screening criteria for blunt cerebrovascular injuries compared with liberal state of the art computed tomography angiography in major trauma. J Trauma Acute Care Surg 2020, 88 (6), 789-795. DOI: 10.1097/ta.0000000000002682 From NLM.
(33) Shiroff, A. M.; Gale, S. C.; Martin, N. D.; Marchalik, D.; Petrov, D.; Ahmed, H. M.; Rotondo, M. F.; Gracias, V. H. Penetrating neck trauma: a review of management strategies and discussion of the ‘No Zone’ approach. Am Surg 2013, 79 (1), 23-29. DOI: 10.1177/000313481307900113 From NLM.
(34) Filler, L.; Akhter, M.; Nimlos, P. Evaluation and Management of the Emergency Department Headache. Semin Neurol 2019, 39 (1), 20-26. DOI: 10.1055/s-0038-1677023 From NLM.
(35) Alons, I. M.; van den Wijngaard, I. R.; Verheul, R. J.; Lycklama à Nijeholt, G.; Wermer, M. J.; Algra, A.; Jellema, K. The value of CT angiography in patients with acute severe headache. Acta Neurol Scand 2015, 131 (3), 164-168. DOI: 10.1111/ane.12302 From NLM.
(36) Han, A.; Yoon, D. Y.; Kim, E. S.; Kim, H. C.; Cho, B. M.; Lee, J. Y. Value of CT angiography for the detection of intracranial vascular lesions in patients with acute severe headache. Eur Radiol 2013, 23 (6), 1443-1449. DOI: 10.1007/s00330-012-2751-4 From NLM.
(37) Alons, I. M. E.; Goudsmit, B. F. J.; Jellema, K.; van Walderveen, M. A. A.; Wermer, M. J. H.; Algra, A. Yield of Computed Tomography (CT) Angiography in Patients with Acute Headache, Normal Neurological Examination, and Normal Non Contrast CT: A Meta-Analysis. J Stroke Cerebrovasc Dis 2018, 27 (4), 1077-1084. DOI: 10.1016/j.jstrokecerebrovasdis.2017.11.016 From NLM.
(38) Rinkel, G. J.; Djibuti, M.; Algra, A.; van Gijn, J. Prevalence and risk of rupture of intracranial aneurysms: a systematic review. Stroke 1998, 29 (1), 251-256. DOI: 10.1161/01.str.29.1.251 From NLM.
(39) Unruptured intracranial aneurysms–risk of rupture and risks of surgical intervention. N Engl J Med 1998, 339 (24), 1725-1733. DOI: 10.1056/nejm199812103392401 From NLM.
(40) Hoh, B. L.; Ko, N. U.; Amin-Hanjani, S.; Chou, S.-Y.; Cruz-Flores, S.; Dangayach, N. S.; Derdeyn, C. P.; Du, R.; Hänggi, D.; Hetts, S. W.; et al. 2023 Guideline for the Management of Patients With Aneurysmal Subarachnoid Hemorrhage: A Guideline From the American Heart Association/American Stroke Association. Stroke 2023, 54 (7), e314-e370. DOI: 10.1161/str.0000000000000436 From NLM.
(41) Thomas, L. E.; Czuczman, A. D.; Boulanger, A. B.; Peak, D. A.; Miller, E. S.; Brown, D. F.; Marill, K. A. Low risk for subsequent subarachnoid hemorrhage for emergency department patients with headache, bloody cerebrospinal fluid, and negative findings on cerebrovascular imaging. J Neurosurg 2014, 121 (1), 24-31. DOI: 10.3171/2014.3.Jns132239 From NLM.
(42) Meurer, W.; Walsh, B. CTA of the Brain is a Reasonable Option to Consider to Help Rule out Subarachnoid Hemorrhage in Select Patients; AAEM, 2014. https://apps.aaem.org/UserFiles/CTAtoHelpRuleOurSubarachnoidHemorrhage.pdf.
(43) Thompson, B. G.; Brown, R. D.; Amin-Hanjani, S.; Broderick, J. P.; Cockroft, K. M.; Connolly, E. S.; Duckwiler, G. R.; Harris, C. C.; Howard, V. J.; Johnston, S. C.; et al. Guidelines for the Management of Patients With Unruptured Intracranial Aneurysms. Stroke 2015, 46 (8), 2368-2400. DOI: doi:10.1161/STR.0000000000000070.
(44) Malhotra, A.; Wu, X.; Geng, B.; Hersey, D.; Gandhi, D.; Sanelli, P. Management of Small Unruptured Intracranial Aneurysms: A Survey of Neuroradiologists. AJNR Am J Neuroradiol 2018, 39 (5), 875-880. DOI: 10.3174/ajnr.A5631 From NLM.
(45) Malhotra, A.; Wu, X.; Forman, H. P.; Matouk, C. C.; Gandhi, D.; Sanelli, P. Management of Tiny Unruptured Intracranial Aneurysms: A Comparative Effectiveness Analysis. JAMA Neurol 2018, 75 (1), 27-34. DOI: 10.1001/jamaneurol.2017.3232 From NLM.
(46) Luttrull, M. D.; Boulter, D. J.; Kirsch, C. F. E.; Aulino, J. M.; Broder, J. S.; Chakraborty, S.; Choudhri, A. F.; Ducruet, A. F.; Kendi, A. T.; Lee, R. K.; et al. ACR Appropriateness Criteria® Acute Mental Status Change, Delirium, and New Onset Psychosis. Journal of the American College of Radiology 2019, 16 (5, Supplement), S26-S37. DOI: https://doi.org/10.1016/j.jacr.2019.02.024.
(47) Smith, A. T.; Han, J. H. Altered Mental Status in the Emergency Department. Semin Neurol 2019, 39 (1), 5-19. DOI: 10.1055/s-0038-1677035 From NLM.
(48) Acharya, R.; Kafle, S.; Shrestha, D. B.; Sedhai, Y. R.; Ghimire, M.; Khanal, K.; Malla, Q. B.; Nepal, U.; Shrestha, R.; Giri, B. Use of Computed Tomography of the Head in Patients With Acute Atraumatic Altered Mental Status: A Systematic Review and Meta-analysis. JAMA Netw Open 2022, 5 (11), e2242805. DOI: 10.1001/jamanetworkopen.2022.42805 From NLM.
(49) Miller, T. H.; Kruse, J. E. Evaluation of syncope. Am Fam Physician 2005, 72 (8), 1492-1500. From NLM.
(50) Langer-Gould, A. M.; Anderson, W. E.; Armstrong, M. J.; Cohen, A. B.; Eccher, M. A.; Iverson, D. J.; Potrebic, S. B.; Becker, A.; Larson, R.; Gedan, A.; et al. The American Academy of Neurology’s top five choosing wisely recommendations. Neurology 2013, 81 (11), 1004-1011. DOI: 10.1212/WNL.0b013e31828aab14 From NLM.
(51) Cornelius, J. F.; Pop, R.; Fricia, M.; George, B.; Chibbaro, S. Compression Syndromes of the Vertebral Artery at the Craniocervical Junction. Acta Neurochir Suppl 2019, 125, 151-158. DOI: 10.1007/978-3-319-62515-7_22 From NLM.
(52) Sun, J.; Zhang, C.; Liu, B.; Li, Y.; Zhang, T.; Tian, J.; Hongyan, B. Eagle Syndrome with Internal Carotid Artery Compression Causing Recurred Syncope. Intern Med 2023, 62 (7), 1067-1071. DOI: 10.2169/internalmedicine.9567-22 From NLM.
(53) Kim, J. S.; Newman-Toker, D. E.; Kerber, K. A.; Jahn, K.; Bertholon, P.; Waterston, J.; Lee, H.; Bisdorff, A.; Strupp, M. Vascular vertigo and dizziness: Diagnostic criteria. J Vestib Res 2022, 32 (3), 205-222. DOI: 10.3233/ves-210169 From NLM.
(54) Du, E. H.; Tenenbaum, M. N.; Bhadelia, R. A.; Sotman, T. E.; Edlow, J. A.; Selim, M. H.; Chang, Y. M. Major radiological outcomes of CTA head and neck performed for dizziness in a major academic Emergency Department. Neuroradiol J 2023, 36 (3), 259-266. DOI: 10.1177/19714009221124304 From NLM.
(55) Searls, D. E.; Pazdera, L.; Korbel, E.; Vysata, O.; Caplan, L. R. Symptoms and signs of posterior circulation ischemia in the new England medical center posterior circulation registry. Arch Neurol 2012, 69 (3), 346-351. DOI: 10.1001/archneurol.2011.2083 From NLM.
(56) Schulz, U. G.; Fischer, U. Posterior circulation cerebrovascular syndromes: diagnosis and management. J Neurol Neurosurg Psychiatry 2017, 88 (1), 45-53. DOI: 10.1136/jnnp-2015-311299 From NLM.
(57) Fakhran, S.; Alhilali, L.; Branstetter, B. F. t. Yield of CT angiography and contrast-enhanced MR imaging in patients with dizziness. AJNR Am J Neuroradiol 2013, 34 (5), 1077-1081. DOI: 10.3174/ajnr.A3325 From NLM.
(58) Edlow, J. A.; Carpenter, C.; Akhter, M.; Khoujah, D.; Marcolini, E.; Meurer, W. J.; Morrill, D.; Naples, J. G.; Ohle, R.; Omron, R.; et al. Guidelines for reasonable and appropriate care in the emergency department 3 (GRACE-3): Acute dizziness and vertigo in the emergency department. Acad Emerg Med 2023, 30 (5), 442-486. DOI: 10.1111/acem.14728 From NLM.
(59) Fonseca, A. C.; Merwick, Á.; Dennis, M.; Ferrari, J.; Ferro, J. M.; Kelly, P.; Lal, A.; Ois, A.; Olivot, J. M.; Purroy, F. European Stroke Organisation (ESO) guidelines on management of transient ischaemic attack. Eur Stroke J 2021, 6 (2), Clxiii-clxxxvi. DOI: 10.1177/2396987321992905 From NLM.
(60) Radiology, A. C. o. ACR Manual on Contrast Media; Media, A. C. o. D. a. C., Ed.; 2023.
(61) Hsieh, C.; Wu, S. C.; Kosik, R. O.; Huang, Y. C.; Chan, W. P. Pharmacological Prevention of Hypersensitivity Reactions Caused by Iodinated Contrast Media: A Systematic Review and Meta-Analysis. Diagnostics (Basel) 2022, 12 (7). DOI: 10.3390/diagnostics12071673 From NLM.
(62) ACR–ASNR–SPR PRACTICE PARAMETER FOR THE PERFORMANCE AND INTERPRETATION OF CERVICOCEREBRAL COMPUTED TOMOGRAPHY ANGIOGRAPHY (CTA). https://www.acr.org/-/media/ACR/Files/Practice-Parameters/CervicoCerebralCTA.pdf (accessed July 16, 2023).
(63) Davenport, M. S.; Perazella, M. A.; Yee, J.; Dillman, J. R.; Fine, D.; McDonald, R. J.; Rodby, R. A.; Wang, C. L.; Weinreb, J. C. Use of Intravenous Iodinated Contrast Media in Patients with Kidney Disease: Consensus Statements from the American College of Radiology and the National Kidney Foundation. Radiology 2020, 294 (3), 660-668. DOI: 10.1148/radiol.2019192094 From NLM.
(64) Bartels, E. D.; Brun, G. C.; Gammeltoft, A.; GjØRup, P. A. Acute anuria following intravenous pyelography in a patient with myelomatosis. Acta Med Scand 1954, 150 (4), 297-302. DOI: 10.1111/j.0954-6820.1954.tb18632.x From NLM.
(65) Solomon, R. Contrast media: are there differences in nephrotoxicity among contrast media? Biomed Res Int 2014, 2014, 934947. DOI: 10.1155/2014/934947 From NLM.
(66) Kinnison, M. L.; Powe, N. R.; Steinberg, E. P. Results of randomized controlled trials of low-versus high-osmolality contrast media. Radiology 1989, 170 (2), 381-389. DOI: 10.1148/radiology.170.2.2643140 From NLM.
(67) Alexopoulos, E.; Spargias, K.; Kyrzopoulos, S.; Manginas, A.; Pavlides, G.; Voudris, V.; Lerakis, S.; McLean, D. S.; Cokkinos, D. V. Contrast-induced acute kidney injury in patients with renal dysfunction undergoing a coronary procedure and receiving non-ionic low-osmolar versus iso-osmolar contrast media. Am J Med Sci 2010, 339 (1), 25-30. DOI: 10.1097/MAJ.0b013e3181c06e70 From NLM.
(68) Lee, T.; Kim, W. K.; Kim, A. J.; Ro, H.; Chang, J. H.; Lee, H. H.; Chung, W.; Jung, J. Y. Low-Osmolar vs. Iso-Osmolar Contrast Media on the Risk of Contrast-Induced Acute Kidney Injury: A Propensity Score Matched Study. Front Med (Lausanne) 2022, 9, 862023. DOI: 10.3389/fmed.2022.862023 From NLM.
(69) McDonald, J. S.; McDonald, R. J.; Comin, J.; Williamson, E. E.; Katzberg, R. W.; Murad, M. H.; Kallmes, D. F. Frequency of acute kidney injury following intravenous contrast medium administration: a systematic review and meta-analysis. Radiology 2013, 267 (1), 119-128. DOI: 10.1148/radiol.12121460 From NLM.
(70) McDonald, J. S.; McDonald, R. J.; Carter, R. E.; Katzberg, R. W.; Kallmes, D. F.; Williamson, E. E. Risk of intravenous contrast material-mediated acute kidney injury: a propensity score-matched study stratified by baseline-estimated glomerular filtration rate. Radiology 2014, 271 (1), 65-73. DOI: 10.1148/radiol.13130775 From NLM.
(71) McDonald, J. S.; McDonald, R. J.; Lieske, J. C.; Carter, R. E.; Katzberg, R. W.; Williamson, E. E.; Kallmes, D. F. Risk of Acute Kidney Injury, Dialysis, and Mortality in Patients With Chronic Kidney Disease After Intravenous Contrast Material Exposure. Mayo Clin Proc 2015, 90 (8), 1046-1053. DOI: 10.1016/j.mayocp.2015.05.016 From NLM.
(72) Ehrmann, S.; Quartin, A.; Hobbs, B. P.; Robert-Edan, V.; Cely, C.; Bell, C.; Lyons, G.; Pham, T.; Schein, R.; Geng, Y.; et al. Contrast-associated acute kidney injury in the critically ill: systematic review and Bayesian meta-analysis. Intensive Care Med 2017, 43 (6), 785-794. DOI: 10.1007/s00134-017-4700-9 From NLM.
(73) Hinson, J. S.; Al Jalbout, N.; Ehmann, M. R.; Klein, E. Y. Acute kidney injury following contrast media administration in the septic patient: A retrospective propensity-matched analysis. J Crit Care 2019, 51, 111-116. DOI: 10.1016/j.jcrc.2019.02.003 From NLM.
(74) Fang, H.; Song, Y. L.; Li, X. S.; Bi, Y. M.; Wang, P.; Fan, H. X.; Meng, L. M.; Hu, H. X. Right arm injection of contrast medium reduces venous artifacts in head and neck multislice spiral computed tomography angiography. Eur Rev Med Pharmacol Sci 2015, 19 (24), 4698-4702. From NLM.
(75) Vertemati, M.; Rizzetto, F.; Cassin, S.; Zerbi, P.; Giordano, A.; Cariati, M.; Gallieni, M. Clinical relevance of the left brachiocephalic vein anatomy for vascular access in dialysis patients. Clinical Anatomy 2020, 33 (8), 1120-1129. DOI: https://doi.org/10.1002/ca.23549.





