Authors: Sheila Goertemoeller, PharmD, DABAT (Clinical Toxicologist, Cincinnati Drug and Poison Information Center, Cincinnati, OH); Shan Yin, MD, MPH (Medical Director, Cincinnati Drug and Poison Information Center, Cincinnati, OH) // Reviewed by: Anthony Spadaro, MD (@TSpadaro91, Medical Toxicology Fellow, Rutgers New Jersey Medical School, Newark, NJ) James Dazhe Cao, MD (@JamesCaoMD, Associate Professor of EM, Medical Toxicology, UT Southwestern Medical Center, Dallas, TX); Alex Koyfman, MD (@EMHighAK); Brit Long, MD (@long_brit)

Case:
A 16-year-old with a history of depression non-compliant of her citalopram was found unresponsive in a dry bathtub with agonal breathing and a weak pulse. When emergency medical services (EMS) arrived, she was in asystole with an empty, recently full, bottle of benzonatate 100 mg capsules. She received cardiopulmonary resuscitation (CPR) and standard advanced cardiovascular life support (ACLS). She had return of spontaneous resuscitation (ROSC) and was subsequently intubated and transported to the emergency department (ED).
Upon ED arrival, she had a heart rate (HR) of 160 and blood pressure (BP) of 80s/40s. Her electrocardiogram (ECG) showed atrial fibrillation which was cardioverted to sinus rhythm. Her QRS interval was 90 and QTc was 491.
Questions:
- What is benzonatate’s mechanism of action?
- What are the signs and symptoms of benzonatate toxicity?
- How quickly can morbidity occur with benzonatate?
- What are the treatment options for a benzonatate overdose?
Background:
- Cough is a frequent complaint that leads to over 20 million annual visits to providers for management.(1)
- There are a limited number of antitussives on the US market which include benzonatate, codeine, dextromethorphan, diphenhydramine, and hydrocodone.
- The US Food and Drug Administration (FDA) approved benzonatate in 1958 for cough relief in patients ≥ 10 years.
- It is currently the only prescription non-narcotic antitussive both widely and increasingly prescribed despite its inferior cough reduction efficacy.(2)
- It is available in an enticing, gold liquid filled, spherical, gelatin capsule under the brand name Tessalon® Perles or in generic preparations.
- It is available in 100 or 200 mg capsules, with a maximum daily dose of 600 mg.
- Benzonatate contains nine ethoxy units, bears molecular resemblance to the local anesthetic tetracaine, and is thought to act similar to a local anesthetic.(3, 4, 5)
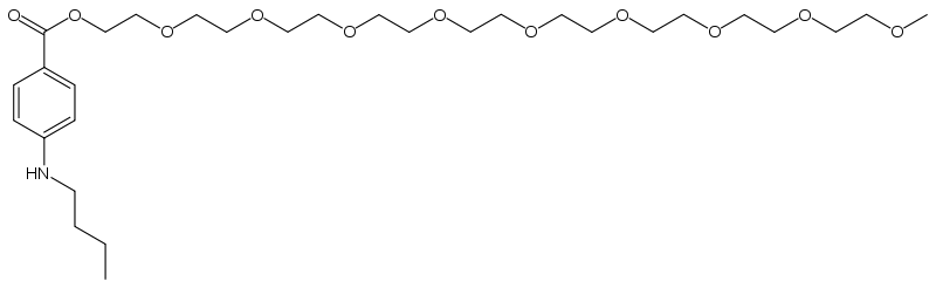
Structure of Benzonatate: Image Courtesy of Wikimedia Commons
- Chemically known as 4-(butylamino) benzoic acid, benzonatate works peripherally anesthetizing the vagal stretch receptors that initiate the cough reflex in the respiratory passages, and centrally in the medulla’s cough center.(6)
- As a local anesthetic it has potent voltage-gated sodium channel-blocking properties.
- It is rapidly absorbed with an onset of 15-20 minutes and duration of up to 8 hours.(7)
Overdose literature review timeline:
- In 1986, the first two benzonatate fatalities were reported in the literature: a choking infant and an intentional overdose in a teenager.(8)
- Over the next 24 years, numerous peer reviewed publications on benzonatate poisoning appeared in the medical literature.(3, 7)
- The accumulating post marketing adverse event reports led to the FDA release of a Drug Safety Communication (DSC) in 2010, over 50 years after initial approval.(9) The safety announcement highlighted the mortality risk of exploratory ingestions in children under 10 years.
- A 2020 National Poison Data System (NPDS) study comparing pre-DSC and post-DSC benzonatate poisonings showed no decrease in the severity nor incidence of benzonatate poisonings reported to US poison control centers.(1)
Epidemiology:
-
- Benzonatate, a non-opioid antitussive, has become a more desirable therapeutic option in the setting of the current opioid epidemic.(5)
- From 2012 to 2019, pediatric benzonatate prescribing soared by 62%.(9)
- In 2019, benzonatate accounted for ~ 10% of all pediatric antitussive prescriptions dispensed via retail pharmacies.(9)
Clinical Presentation:
- Clinical symptoms are mostly related to its sodium channel blocking propensity which result in neurologic and cardiovascular toxicity.
- Neurologic symptoms: Encephalopathy, seizures, or coma(5,7)
- Cardiovascular symptoms: Hypotension, conduction disturbances, ventricular tachycardia or fibrillation, pulseless electrical activity, or asystole(10)
- Breaking, crushing, or chewing the capsules can produce numbness, choking, bronchospasm or laryngospasm.(5)
- Patients who survive may have permanent end organ damage including neurologic deficits.
- Most pediatric and adult benzonatate case reports have ill-defined toxic dose ranges.
- A child died from as little as 400 mg while an adult survived a 3600 mg ingestion.(10)
- A systematic review of severe benzonatate poisonings published in 2021 demonstrated survival in greater than 60% of patients.(10)
Diagnosis:
- Benzonatate poses both diagnostic and analytical challenges.
- There is no specific toxidrome nor pathognomonic signs attributable to benzonatate.
- High performance liquid chromatography (HPLC) is possible for quantitative analysis; however, most hospitals do not have it readily available and is unlikely to result in a clinically relevant timeframe.
Management:
- The mainstay of treatment of benzonatate overdose is supportive and symptomatic care.
- It is important to pay particular attention to airway, breathing, and circulation (ABCs).
- For severe toxicity a toxicologist should be consulted early in the course.
- There is no specific antidote for benzonatate.
- Activated charcoal can be considered if patients present shortly after overdose and are without risk for aspiration.
- Benzodiazepines are first-line therapy for seizures.
- For QRS prolongation (>100 msec), 1-2 mEq/kg of sodium bicarbonate boluses and reassessment of the QRS interval should be considered.
- For hypotension, intravenous fluids are first line, followed by vasopressors as necessary.
- Intravenous lipid emulsion (ILE) can be used for life-threatening local anesthetic toxicity.(11)
- A bolus dose at 1.5 mL/kg of 20% intravenous lipid emulsion given over 1 minute followed by an infusion at 0.25 mL/kg/min to a maximum infusion of 10 mL/kg over 30-60 minutes.(11) Prolonged infusion of ILE may be harmful and a toxicologist should be consulted for the use of ILE infusions.(11)
- Benzonatate does not have intrinsically favorable lipophilicity for ILE, however it has been used successfully in some case reports.(10)
Case Follow-up:
Over the course of 2 days on the pediatric intensive care unit (PICU) the patient developed multiple myoclonic seizures that did not respond to benzodiazepines nor levetiracetam. A computed tomography (CT) showed diffuse loss of gray-white matter differentiation with evidence of cerebral edema marked by hemispheric sulcal effacement and early trans tentorial herniation consistent with global hypoxic ischemic injury. Five days after the overdose the patient stopped initiating breaths on the ventilator, became hypotensive and had no brain activity. Care was withdrawn and she progressed to asystole and death. The coroner report ruled her death as hypoxic-ischemic encephalopathy of undetermined etiology.
Clinical Pearls:
- Benzonatate is increasingly prescribed as an antitussive.
- It can cause rapid and dramatic neurologic and cardiovascular toxicity, including death.
- There is no specific toxidrome or antidote for a benzonatate overdose.
- Interventions are supportive including benzodiazepines for seizures, sodium bicarbonate for prolonged QRS and arrhythmias, and intravenous lipid emulsion for cardiac arrest.
References:
- Leonard JB, Seung H, Klein-Schwartz W. Impact of a drug safety communication on the severity of benzonatate exposures reported to poison centers. Pharmacoepidemiol Drug Saf. 2021;30(1):45-52. Epub 20200923. doi: 10.1002/pds.5136. PubMed PMID: 32964590.
- Stephens RJ, Filip AB, Baumgartner KT, Schwarz ES, Liss DB. Benzonatate Overdose Presenting as Cardiac Arrest with Rapidly Narrowing QRS Interval. J Med Toxicol. 2022;18(4):344-9. Epub 20220705. doi: 10.1007/s13181-022-00904-4. PubMed PMID: 35790679; PubMed Central PMCID: PMC9492832.
- McLawhorn MW, Goulding MR, Gill RK, Michele TM. Analysis of benzonatate overdoses among adults and children from 1969-2010 by the United States Food and Drug Administration. Pharmacotherapy. 2013;33(1):38-43. doi: 10.1002/phar.1153. PubMed PMID: 23307543.
- Jin C, Zahid E, Sherazi A, Majumder MR, Bedi P. Cardiac Arrest Due to Benzonatate Overdose. Am J Case Rep. 2019;20:640-2. Epub 20190503. doi: 10.12659/AJCR.915151. PubMed PMID: 31048669; PubMed Central PMCID: PMC6512753.
- Bishop-Freeman SC, Shonsey EM, Friederich LW, Beuhler MC, Winecker RE. Benzonatate Toxicity: Nothing to Cough At. J Anal Toxicol. 2017;41(5):461-3. doi: 10.1093/jat/bkx021. PubMed PMID: 28334901.
- Homsi J, Walsh D, Nelson KA. Important drugs for cough in advanced cancer. Support Care Cancer. 2001;9(8):565-74. doi: 10.1007/s005200100252. PubMed PMID: 11762966.
- Yoshioka I, Surmaitis R, Katz KD. A 17-Year-Old Girl With Cough–Pulseless After Drug Overdose. Sodium benzonatate overdose. Pediatr Emerg Care. 2016;32(3):197-9. doi: 10.1097/PEC.0000000000000733. PubMed PMID: 26928103.
- Cohan JA, Manning TJ, Lukash L, Long C, Ziminski KR, Conradi SE. Two fatalities resulting from Tessalon (benzonatate). Vet Hum Toxicol. 1986;28(6):543-4. PubMed PMID: 3788039.
- Kim I, Goulding M, Tian F, Karami S, Pham T, Cheng C, et al. Benzonatate Exposure Trends and Adverse Events. Pediatrics. 2022;150(6). doi: 10.1542/peds.2022-057779. PubMed PMID: 36377394; PubMed Central PMCID: PMC9732921.
- Minhaj FS, Leonard JB. A description of the clinical course of severe benzonatate poisonings reported in the literature and to NPDS: A systematic review supplemented with NPDS cases. Hum Exp Toxicol. 2021;40(12_suppl):S39-S48. Epub 20210705. doi: 10.1177/09603271211030560. PubMed PMID: 34219543.
- American College of Medical Toxicology. ACMT Position Statement: Guidance for the Use of Intravenous Lipid Emulsion [published correction appears in J Med Toxicol. 2016 Dec;12 (4):416]. J Med Toxicol. 2017;13(1):124-125. doi:10.1007/s13181-016-0550-





