Author: Adam Lalley, MD (EM Resident Physician, Maimonides Medical Center, Brooklyn, NY) // Reviewed by: Mark Ramzy, DO (@MRamzyDO); Alex Koyfman, MD (@EMHighAK); Brit Long, MD (@long_brit)
Introduction
From the poles that hang from ED ceilings and rise from the backs of stretchers, intravenous (IV) fluids are a hallmark of hospital and pre-hospital care. They’re part of the backbone of treatment for conditions like DKA and gastroenteritis. Used liberally for the irrigation of lacerations and chemical eye injuries, they can even be found in supply closets beside wound dressings, hydrogen peroxide, and bacitracin.
A growing body of research has aimed to refine the use, selection, and overall duration of IV fluids. This article explores recent literature from a variety of disciplines – including the most updated guidelines for the management of trauma and sepsis – that highlight instances in which normal saline or other crystalloids should not be the norm.
Cardiovascular and Cardiopulmonary Systems
Case: 74-year-old woman and active smoker with a past medical history of hypertension, Type II diabetes mellitus, COPD, and breast cancer resected 20 years ago presents to the Emergency Department with 3 days of worsening chest pain. She attests to dyspnea and near-syncope on exertion. Her symptoms are not associated with fevers, diaphoresis, abdominal pain, vomiting, or dysuria. The patient does not use supplemental oxygen at home.
Vital signs include HR 123, BP 100/62, SpO2 86%, RR 32, Temp 98.9 F. Exam reveals a listless, cyanotic, obese woman with cool extremities. Lungs are rhonchorous with diffuse wheezing but no rales. With O2 via a non-rebreather, vital signs improve to HR 95, BP 102/64, SpO2 92% RR 26. BUN and creatinine are increased to 35/1.8 from a baseline of 20/1.0. EKG shows right axis deviation but no other signs of ischemia. Chest x-ray reveals increased lung volumes. A CT chest with contrast is unremarkable, but the patient remains persistently dyspneic and hypoxic. She continues to improve with non-invasive ventilation, albuterol/ipratropium nebulization, and steroids. The patient is admitted to observation, where a formal echocardiogram reveals poor right ventricular function with bowing of the interventricular septum into the left ventricle.
Discussion:
This patient presented with a COPD exacerbation complicated by acute-on-chronic pulmonary hypertension and right heart failure.
The dyspnea she reports is the most common symptom of pulmonary hypertension,1 a condition that is frequently left off the differential in emergency departments.2 Chest pain is another common symptom of pulmonary hypertension, and it is thought to stem from demand ischemia in a right ventricle that has become so hypertrophied that its own perfusion is impaired.1,3 In the most severe cases, patients may experience exertional syncope or pre-syncope due to the finite, decreased cardiac output that results. 1,3
Additional exam findings of pulmonary hypertension with right heart failure can include hypotension, diaphoresis, cyanosis, and tachycardia.4 Less commonly, patients may report discomfort in the right upper quadrant from congestive venous distension of the hepatic capsule.4 When the left ventricle is not involved (i.e., in isolated right heart failure), lungs are typically clear to auscultation, even in the worst cases.3
COPD is the most frequent cause of chronic pulmonary hypertension,3 which often progresses to chronic right heart failure.4 Other precursors of chronic right heart failure include primary cardiomyopathies with right ventricular involvement and valvular pathologies.4 Obstructive sleep apnea and obesity hypoventilation syndrome are increasingly common predisposing factors.3 The more acute causes include disorders that either increase right ventricular afterload or reduce contractility, such as pulmonary emboli, right ventricular ischemia, and myocarditis.4
The prevailing cause of right heart failure overall is left heart failure,3 where fluid overload can declare itself with pulmonary edema.5 In these cases, there are often clear signs that fluid should be given gently, if at all (i.e., crackles on lung exam or radiographic/sonographic evidence of congestion).5 To contrast isolated right heart failure from isolated left heart failure, it is sometimes taught that right heart failure is “preload dependent.” However, this adage is overly reductionist,4 and a review of right heart physiology is needed before we hang a bag of fluids.
When pulmonary resistance increases (as in pulmonary hypertension or pulmonary emboli), it inhibits right ventricular output, leading to a pooling of volume in the right ventricle.3 When the compliance of the right ventricle can no longer accommodate this volume, the interventricular septum deviates into the left ventricular space, reducing left ventricular filling and thus overall cardiac output – a phenomenon referred to as interventricular interdependence.3,4
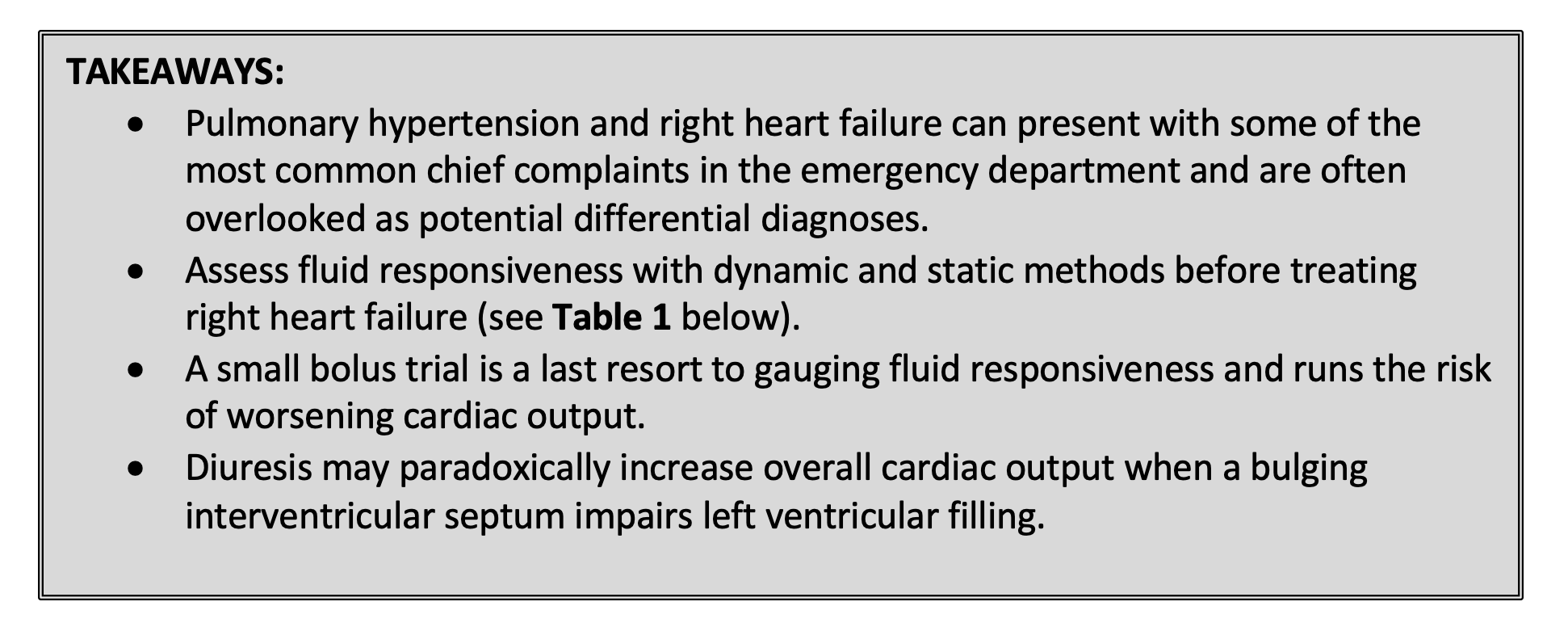
This pathologic distension of the right ventricle, in which an encroaching interventricular septum steals real estate from its neighboring left ventricle, is a more prominent culprit of decreased cardiac output than reduced right ventricular preload.4 Until we figure out the cause of low cardiac output, it may be helpful to first consider static or dynamic assessments of fluid responsiveness (see Table 1 below), with perhaps a small fluid bolus trial as a last resort.4 Too much preload runs the risk of worsening the clinical picture if it dilates an already thin-walled right ventricle that is pushing blood uphill against an insurmountable afterload.4 In these cases, the solution to augmenting output may instead lie in diuresis.4
The right ventricular “spiral of death” is rooted in its particular pattern of coronary perfusion. Unlike the left ventricle, which is perfused primarily during diastole when the myocardium relaxes, the right ventricle’s relatively lower wall tension allows perfusion during both relaxation and contraction.3,4 However, when right ventricular afterload increases, distension can increase the wall stress beyond the limit of perfusion. The right ventricle becomes ischemic, further damaging its ability to squeeze, which in turn worsens distension3,4 and coronary congestion.4
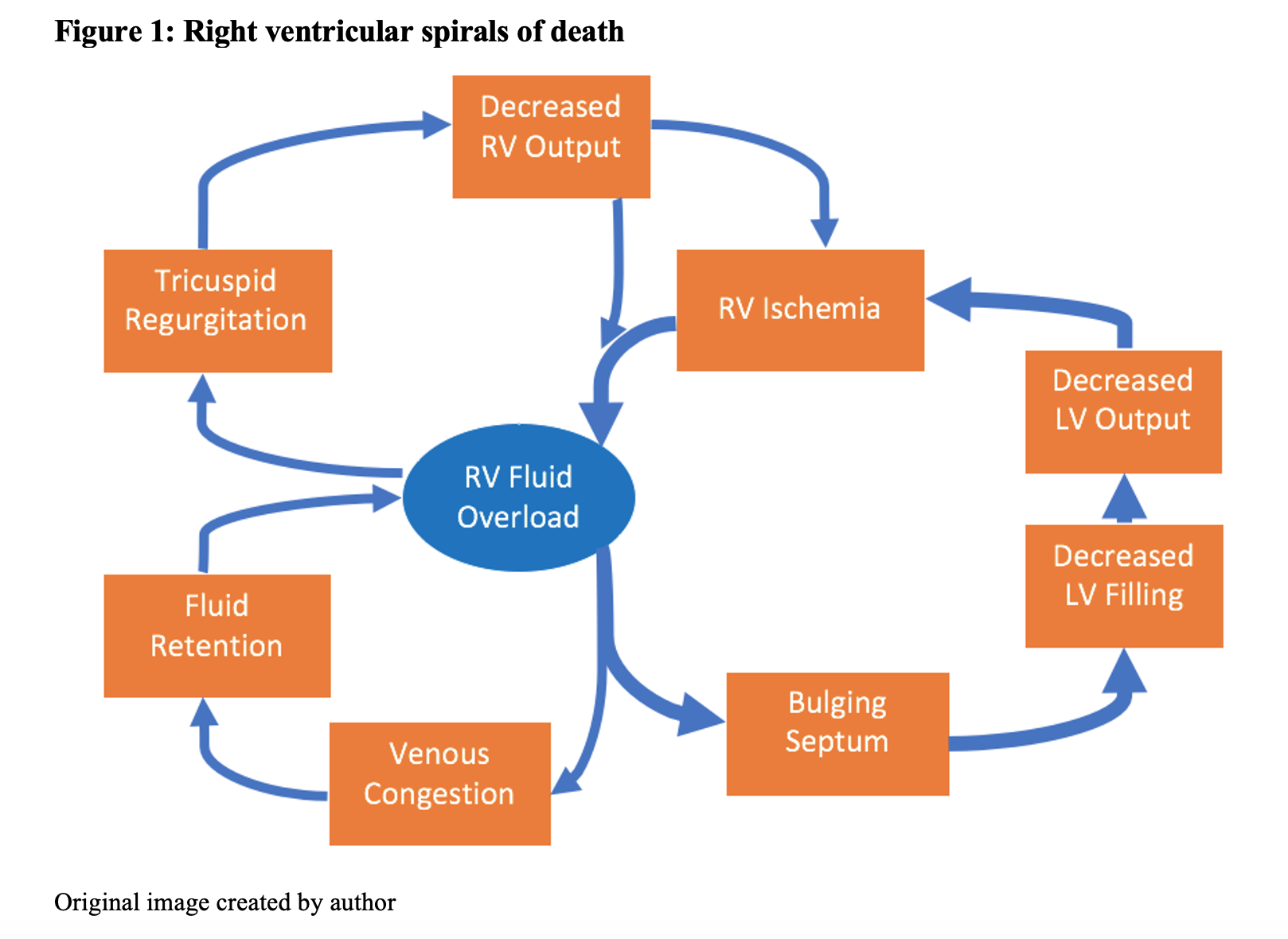
To make matters worse, venous congestion in the liver and kidneys from gridlock in the right ventricle further exacerbates fluid retention by hampering the ability of these organs to offload excess volume,4 which in turn perpetuates right ventricular overload.
In short, right heart dysfunction is a potentially fatal disease that can be tricky to diagnose in the acute setting of the emergency department. It has been shown to be an independent predictor of increased mortality for patients with dyspnea6 and a frequent cause of both repeat testing and ICU admission.2 In many of these cases, fluids won’t put out the fire; they may just add fuel.
Renal
Case: A 54-year-old undomiciled woman with a history of intravenous drug and alcohol use disorder presents with decreased appetite, abdominal distension, diarrhea, and weakness. She denies fevers, chills, chest pain, shortness of breath, dysuria, hematuria, and vaginal bleeding.
Initial vital signs include HR 108, BP 98/46, RR 20, SpO2 95%, Temp 97.2 F. Exam reveals a tired-appearing woman, alert and oriented, with scleral icterus. Her cardiopulmonary exam is normal, but she has a distended, non-tender abdomen. Labs show hyponatremia, elevated BUN with a doubling of her creatinine compared to an admission a year ago. Transaminases are markedly elevated with hypoalbuminemia and bilirubinemia. A hepatitis panel reveals antibodies to hepatitis C.
Discussion:
This patient has pre-renal acute kidney injury (AKI), likely due to cirrhosis from hepatitis C. Acute kidney injury is an abrupt decline in kidney function triggered by two broad categories of renal ischemia: 1) selectively decreased blood flow to the kidneys or 2) systemic hypoperfusion. Of note, though hypovolemia can cause hypoperfusion (as in hemorrhagic shock or severe gastrointestinal losses), hypoperfusion has other causes and may be unrelated to volume status. For example, in septic shock, cardiac shock, heart failure, or cirrhosis, patients can suffer from decreased renal perfusion in the setting of total body edema. In these circumstances, injudicious use of IV fluids can worsen renal injury.
In fluid overload, increased interstitial edema within the confines of renal capsules leads to reduced filtration7,8 due to both decreased venous/lymphatic outflow and attenuated arterial inflow.8 In animal models, thirty minutes of venous congestion from clamping of the renal vein alone (as opposed to clamping of the renal artery alone or both the renal vein and artery together) has been shown to decrease blood flow and increase creatinine more than the same duration of renal artery clamping.9
Fluid overload has been correlated with increased mortality in the critically ill5 and in post-surgical patients, independently of the type of fluid employed.10 Table 1 provides an overview of methods that emergency physicians can use to assess a patient’s fluid status. It should be noted that fluid overload may be a marker of severe disease rather than, or in addition to, a cause of it.11 That said, attention has focused on exploring the potential benefits of restrictive or conservative fluid treatment strategies, not only to reduce volume loads but also to mitigate the burden on kidneys of supra-physiologic electrolyte levels.

Compared to balanced crystalloids (i.e., lactated Ringers or Plasmalyte), sodium chloride has been shown to increase interstitial edema and trigger more adverse microvascular effects, including decreased renal cortical blood flow and oxygen delivery.8 The SALT-ED trial found no difference in hospital-free days between the balanced crystalloid and normal saline groups, but the sodium chloride group did experience a higher incidence of major adverse kidney events.13 Sodium chloride is well known to run the risk of inducing hyperchloremic metabolic acidosis due to its supra-physiologic levels of chloride,10 but authors have also recently focused on the effects of sodium itself.
Only two liters of lactated Ringer’s contains more sodium than the average daily dietary intake of the country with the highest sodium consumption in the world.10 What’s more, many drugs themselves, particularly antibiotics, feature sodium as a mechanism to dissolve in water for intravenous administration.10 It can take days to excrete these sodium loads. In one trial, after a jump in dietary sodium intake with its associated fluid retention, healthy volunteers took days to lose those additional kilograms of body weight.10
The FRESH trial used passive leg raise in conjunction with dynamic measures of stroke volume to guide a more conservative approach to fluid resuscitation in sepsis-related hypotension.7 The study’s authors found that the gap in fluid balance between the more conservative arm and the standard-of-care arm at 72 hours was not closed by the use of diuretics or dialysis in the control arm.7 Their evidence suggests that the consequences of early fluid administration extend much farther than the emergency department.

Endocrine
Case: 71-year-old active smoker is brought in by his daughter for acutely worsening confusion. The daughter also reports a worsening cough and unintentional weight loss of 10 pounds in the past two months. When asked, the patient endorses some chest discomfort, nausea, malaise, decreased appetite, and headache. Vital signs include temp 98.6 F, HR 80, BP 130/80, RR 18, SpO2 94% on room air. Exam reveals a thin man who is slow to respond to questions but provides appropriate, linear answers. He has an occasional cough but clear lungs on auscultation without wheezing, rales, or rhonchi. There is no appreciable JVD, hepatojugular reflex, or lower extremity pitting edema. Labs are significant for sodium of 120 with a normal glucose. Chest x-ray reveals a mass in the right middle lobe. A liter of normal saline is started with the belief that the patient is hypovolemic and will benefit from sodium supplementation. Serum osmolality later returns at 270 with urine osmoles of 650.
Discussion:
While sodium chloride remains the treatment of choice for hypovolemic hyponatremia,14 the administration of normal saline can be premature for other forms of mild-to-moderate hyponatremia until the fluid status or etiology of hyponatremia are evaluated. This patient is subsequently diagnosed with small cell lung carcinoma complicated by SIADH, which is consistent with euvolemic, hypo-osmolar hyponatremia and concentrated urine.
Despite up-and-coming novel medications, fluid restriction is still the first-line treatment for hyponatremia caused by SIADH.15 Giving 0.9% sodium chloride in the belief that supra-physiologic levels of sodium can only elevate a low serum sodium level will in fact worsen hyponatremia in patients with SIADH.14 The excretion of sodium is intact in these patients, and their kidneys will not re-absorb all of the sodium in intravenous fluids. However, inappropriately high levels of ADH will lead to retention of the free water component in intravenous fluids, resulting in further dilution of electrolytes in circulating blood.14
As with fluid overload, it needs to be said that hyponatremia may also occasionally be more of a marker of severe disease than a cause of it.16 Accordingly, it may make more sense to treat the underlying cause of hyponatremia if it is not the primary disease process. For example, SIADH has a myriad of causes that include malignancy, intracranial pathology, and medications. It is also considered a diagnosis of exclusion that implies otherwise normal function of the kidneys, thyroid, and adrenal systems.14
As for hypervolemic hyponatremia, it is often precipitated by heart failure, cirrhosis, and nephrotic syndrome. In these instances, the kidney senses decreased perfusion and triggers water retention out of proportion to sodium retention, leading to a high volume of fluid in the extra-cellular space.14 Urine sodium is typically < 20mmol/L, and the first-line treatment involves water restriction to 1-1.5 L/day and a low-sodium diet, with second-line treatments involving diuretic use in consultation with cardiology, hepatology, and/or nephrology.14,15
Note that this article does not address the indications for or use of hypertonic saline, nor does it aim to cover hyponatremia in the context of subarachnoid hemorrhage.

Trauma
Case: 22-year-old man is brought in by EMS after bystanders witnessed three assailants attack the patient with knives 20 minutes prior to arrival while the patient was walking along the sidewalk. According to EMS, the patient was found on the ground moaning incomprehensibly in a pool of blood, which they estimate to be about 500 mL. On arrival to the resuscitation bay, the patient’s airway is intact. A partially occlusive dressing has been placed over a sucking chest wound on the left side. A chest tube is placed on the left and oxygen saturations improve from 88% to 95%. A penetrating wound is noted in the right upper quadrant with active oozing beneath a soaked layer of absorbent gauze. A tourniquet has been secured around the right upper extremity above an open laceration through the right antecubital fossa and right distal forearm. EMS obtained IV access, and 0.9% sodium chloride is flowing wide open into the left antecubital fossa and left foot. Manual blood pressure reading is 94/46, down from the most recent EMS measurement of 102/60. Heart rate is 130bpm, increased from 118 prehospital. GCS is 8, and the patient is intubated for airway protection. EFAST exam reveals free fluid in Morrison’s pouch and around the bladder. Massive transfusion protocol is activated, and the patient is taken emergently to the operating room for an exploratory laparotomy.
Discussion:
This patient is in hemorrhagic shock from multiple penetrating injuries, including an actively bleeding abdominal wound without definitive hemorrhage control. Since the 1970s, fluid preferences for the resuscitation of bleeding trauma patients have evolved.17 An initial affinity for whole blood gave way to a recommendation for separated, component blood products.17 Guidelines later favored crystalloids17 combined with aggressive fluid resuscitation targets, including the goal of “supra-normal” cardiac output.18
For trauma patients without significant brain or spinal cord injuries, treatment strategies now emphasize “damage control resuscitation.”17-19 This approach involves controlled volume replacement with a goal of permissive hypotension (i.e., a systolic blood pressure of around 90 mm Hg) until bleeding can be definitively addressed, often with surgical intervention.17-19 Damage control resuscitation has shifted the paradigm away from crystalloids and toward the early use of blood products, ideally in a 1:1:1 ratio of RBCs to platelets to plasma.17
These latest strategies have led to fewer complications of fluid overload, less coagulopathy, and improved survival.20,21By contrast, approaches that raise blood pressure to normal levels run the risk of aggravating hemorrhage, exacerbating coagulopathies, worsening edema, impairing tissue oxygenation,21 dislodging blood clots, and dropping core body temperature.19
Three important recent studies have focused on associations between pre-hospital/emergency medicine resuscitations and the mortality of adult trauma cases. A paper by Brown et al found that adult trauma patients who received >500 ml of crystalloids in the pre-hospital setting suffered significantly increased mortality and a higher INR if they were not already hypotensive.22 For those who were hypotensive, the authors found no difference between patients who received >500 ml fluid and those who received < 500 ml fluid.22
A single-center retrospective trial suggested that crystalloid volume administration as low as 1.5 L in the Emergency Department was also associated with higher mortality in adult trauma patients. While statistical analyses attempted to adjust for differences in injury severity, this study was limited by its retrospective nature.21
Finally, a retrospective cohort analysis found that resuscitation with ≥ 5L crystalloids in the first 24 hours was independently associated with mortality.20 It should be noted that these patients also had a significantly higher injury severity score than those who received less fluid.20 They also had significantly worse baseline physiologic parameters and lab values.20
Though the evidence remains relatively weak, the overall picture suggests that when it comes to crystalloid administration in hemorrhagic shock, less may be more.

Infectious Disease
Case: 79-year-old bedbound woman with a past medical history of type II diabetes, hypertension, coronary artery disease, atrial fibrillation, congestive heart failure, stroke with left-sided residual deficits, and multiple urinary tract infections is sent from her nursing home after staff noticed her slump over her meal. They describe her as more lethargic and confused than usual with increased work of breathing and foul-smelling urine in her diaper. Vitals include temperature of 100.6 F, BP 90/54, HR 119, RR 24, SpO2 91% on 10L non-rebreather placed by EMS. On exam, the patient is ill-appearing and mumbling incoherently with diffuse rales, JVD, and an irregularly irregular cardiac rhythm. Her abdomen is soft, non-tender and non-distended. There is 1+ lower extremity pitting edema. The rest of her exam is unremarkable. Labs reveal leukocytosis of 14k with 12% bands, and urinalysis is positive for leukocyte esterase and nitrates.
Discussion:
This patient presents with all four SIRS criteria with likely infectious sources including a urinary tract infection, pyelonephritis, and/or pneumonia. In short, she has sepsis with hypotension, but she is displaying concomitant signs of fluid overload that could worsen with aggressive intravenous fluid administration.
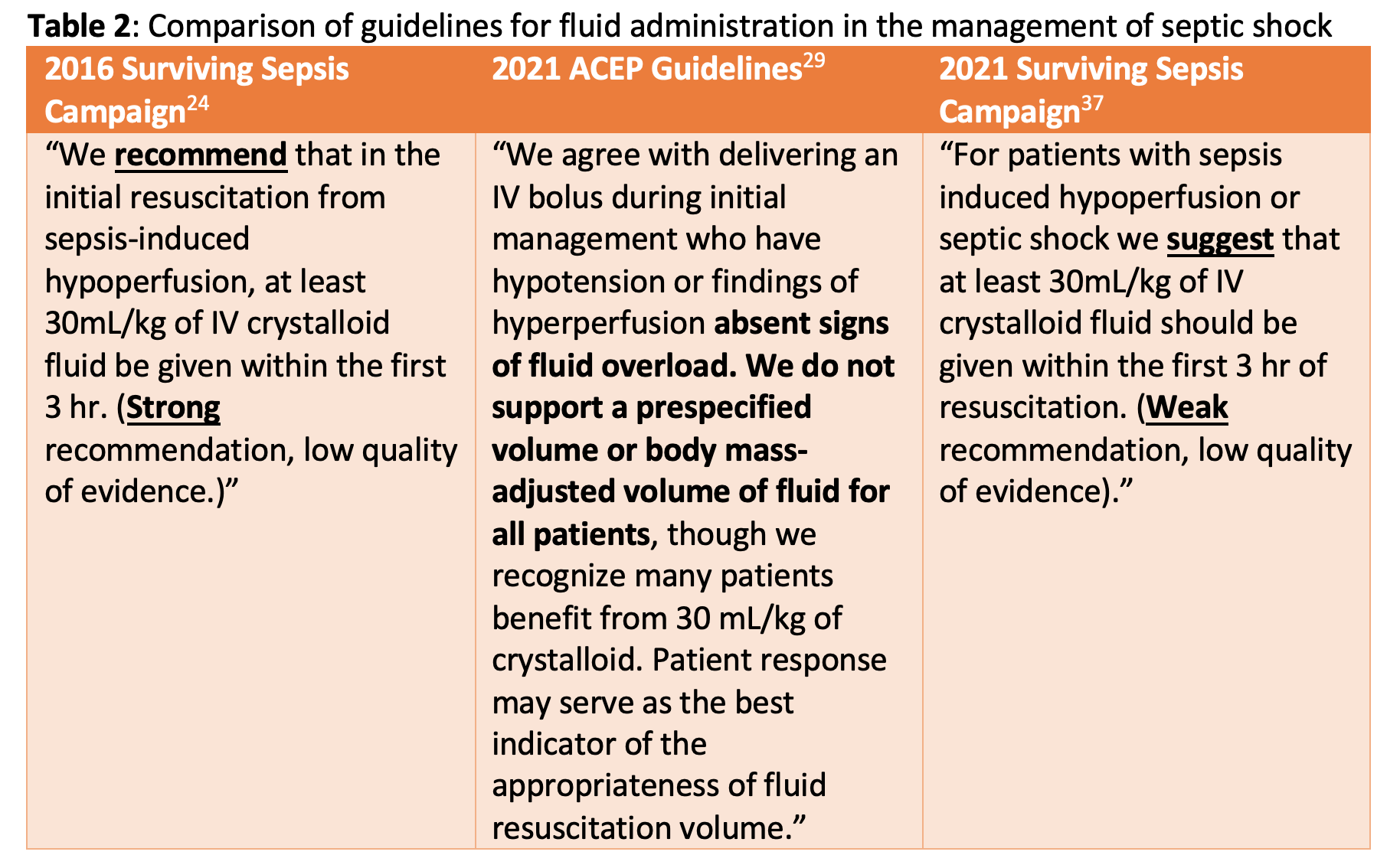
Based on weak evidence, the 2016 Surviving Sepsis Campaign guidelines strongly recommended an initial fixed volume of 30 mL/kg IV crystalloid within the first 3 hours for sepsis-induced hypoperfusion.23 The specific weight-based amount of crystalloid was derived from data in the ProCESS,24 ARISE,25 and ProMISe26 trials, which were consistent with common practice in the emergency departments and ICUs.23 The guidelines were also consistent with the SEP-1 Core Measure from the Centers for Medicare and Medicaid Services and The Joint Commission, which echoed the 30 mL/kg infusion of crystalloids within the first 3 hours of recognizing septic shock.27,28
Recent data, however, have noted that the beneficial hemodynamic effects of fluid boluses are often short-lived.27Boluses can also make matters worse. One observational study revealed that while mortality marginally decreased with each incremental liter of IV fluids up to 5 liters on the first day of treatment, mortality increased with every liter afterwards within the same time period.27
Since the release of the 2016 Sepsis Guidelines, several authors have opposed dogmatic adherence to a flat 30 mL/kg of fluids within the first three hours.11,29-34 They suggest a more individualized and situational approach. Self et al have proposed that a shift toward a more restrictive fluid strategy in septic shock may even parallel the paradigm change toward damage control resuscitation in the treatment of hemorrhagic shock.27 Their multicenter, unblinded, randomized study comparing liberal vs. restrictive approaches to intravenous fluid resuscitation in the first 24 hours of septic shock management for US adults (the Crystalloid Liberal or Vasopressor Early Resuscitation in Sepsis [CLOVERS] trial) is currently underway27 and much anticipated.
In July 2021, the American College of Emergency Physicians (ACEP) released a consensus-based task force report that explicitly states, “we do not support a prespecified volume or body mass-adjusted volume of fluid for all patients” for sepsis-induced hypotension.12 Of note, along with these recommendations, ACEP also supported the use of balanced crystalloid solutions (Ringer’s solution or Plasmalyte) over normal saline in the interest of reducing hyperchloremic metabolic acidosis and impaired renal performance, particularly when more than 1 L is used.12
Just a few months later, in October 2021, the Surviving Sepsis Campaign subsequently downgraded its endorsement of a 30 mL/kg bolus from “strong” to “weak.”35 Among other key revisions, they also altered the verbiage from “recommend” to “suggest” and placed a greater emphasis on the pitfalls of excessive fluid resuscitation, including prolonged ventilation, acute kidney injury, and increased mortality.35

Conclusion:
Fluid overload has been associated with increased post-operative complications and can be detrimental to multiple organ systems, with consequences including poor gas exchange, impaired renal function,13 and slower wound healing.13,20
Given that no ideal fluid exists, recent literature has suggested that physicians should treat crystalloids like any other prescribed drug.18 Some suggest that antibiotic selection might serve as a model.11,16 This framework involves considering the “4 D’s”:
- Drug – consider the side effects of fluids (i.e., hyperchloremic metabolic acidosis) along with their benefits; the patient’s underlying conditions (i.e., kidney disease, heart failure, cirrhosis); the specific use of the fluid (i.e., resuscitation, replacement, maintenance); and the type of fluid that would best suit the patient’s needs.16
- Dosing – consider both the timing and the speed of fluid administration relative to the illness course along with the parameters you might use to monitor the patient’s response.16
- Duration – while the triggers to start fluid therapies are often clear, the triggers to stop them are often less evident. Emergency physicians, especially those in critical care, may benefit from establishing clear goals for fluid tapering.16
- De-escalation – the final step is knowing when to withdraw fluids when resuscitation is no longer required.16
Hopefully, the framework above along with a review of the handful of conditions mentioned in this article can help emergency physicians to think more deliberately about resuscitative strategies. Sometimes it’s all too easy to check that box for fluids and risk rubbing salt into wounds.
References:
- Rich JD, Rich S. Clinical diagnosis of pulmonary hypertension. 2014;130:1820-1830.
- Russell FM, Moore CL, Courtney DM, et al. Independent evaluation of a simple clinical prediction rule to identify right ventricular dysfunction in patients with shortness of breath. Am J Emerg Med. 2015;33:542-547.
- Wilcox S, Kabrhel C, Channick R. Pulmonary hypertension and right ventricular failure in emergency medicine. Ann Emerg Med. 2015;66(6):619-628.
- Konstam M, Kiernan M, Bernstein D. Evaluation and management of right-sided heart failure: a scientific statement from the American Heart Association. Circulation. 2018; 137:e578-e622.
- Claure-Del Granado R, Mehta R. Fluid overload in the ICU: evaluation and management. BMC Nephrology.2016;17:109.
- Chen AA, Wood MJ, Krauser DG, et al. NT-proBNP levels, echocardiographic findings, and outcomes in breathless patients: results from the ProBNP Investigation of Dyspnoea in the Emergency Department (PRIDE) echocardiographic substudy. Eur Heart J. 2006;27:839–45.
- Douglas I, Alapat P, Corl K, et al. Fluid response evaluation in sepsis hypotension and shock: a randomized clinical trial. Chest. 2020;158(4):1431-1445.
- Ding X, Cheng Z, Qian Q. Intravenous fluids and acute kidney injury. Blood Purif. 2017;43:163-172.
- Li X, Liu M, Bedja D, et al. Acute renal venous obstruction is more detrimental to the kidney than arterial occlusion: implication for murine models of acute kidney injury. Am J Physiol Renal Physiol. 2012;302:F519-F525.
- Van Regenmortel N, Moers N, Langer T, et al. Fluid-induced harm in the hospital: look beyond volume and start considering sodium. Intensive Care. 2021;11:79.
- Malbrain M, Langer T, Annane D, et al. Intravenous fluid therapy in the perioperative and critical care setting: executive summary of the International Fluid Academy (IFA). Intensive Care. 2020;10:64.
- Yealy D, Mohr N, Shapiro N, Venkatesh A, Jones A, Self W. Early care of adults with suspected sepsis in the emergency department and out-of-hospital environment: a consensus-based task force. Ann Emerg Med.2021;78(1):1-19.
- Self W, Semler M, Wanderer J, et al. Balanced crystalloids versus saline in noncritically ill adults. N Engl J Med. 2018;378(9):819-828.
- Lee J, Kilonzo K, Nistico A, Yeates K. Management of hyponatremia. CMAJ. 2014;186(8):E281-E286.
- Hoorn E, Spasovski G. Recent developments in the management of acute and chronic hyponatremia. Curr Opin Nephrol Hypertens. 2019;28(5):424-432.
- Malbrain M, Van Regenmortel N, Owczuk R. It is time to consider the four D’s of fluid management. Anaesthesiol Intensive Ther. 2015;47:s1-s5.
- Cannon J, Khan M, Raja A, et al. Damage control resuscitation in patients with severe traumatic hemorrhage. J Trauma. 2017;82(3):605-617.
- Chang R, Holcomb J. Optimal fluid therapy for traumatic hemorrhagic shock. Crit Care Clin. 2017;33(1):15-36.
- Roussaint R, Bouillon B, Cerny V, et al. The European guideline on management of major bleeding and coagulopathy following trauma: fourth edition. Critical Care. 2016;20:100.
- Jones D, Nantais J, Rezende-Neto J, Yazdani S, Vegas P, Rizoli S. Crystalloid resuscitation in trauma patients: deleterious effect of 5L or more in the first 24h. BMC Surgery. 2018;18:93.
- Ley E, Clond M, Srour M, et al. Emergency department crystalloid resuscitation of 1.5L or more is associated with increased mortality in elderly and nonelderly trauma patients. J Trauma Inj Infect Crit Care. 2011;70(2):398-400.
- Brown JB, Cohen MJ, Minei JP, et al. Goal-directed resuscitation in the prehospital setting: a propensity-adjusted analysis. J Trauma Acute Care Surg. 2013; 74(5):1207–1212.
- Rhodes A, Evans L, Alhazzani W, et al. Surviving Sepsis Campaign: international guidelines for management of sepsis and septic shock: 2016. Care Med. 2017;45(3):486-552.
- Yealy DM, Kellum JA, Huang DT, et al: A randomized trial of protocol-based care for early septic shock. N Engl J Med. 2014;370(18): 1683–1693.
- Peake SL, Delaney A, Bailey M, et al: Goal-directed resuscitation for patients with early septic shock. N Engl J Med. 2014;371(16): 1496–1506.
- Mouncey PR, Osborn TM, Power GS, et al; ProMISe Trial Investigators: Trial of early, goal-directed resuscitation for septic shock. N Engl J Med. 2015; 372:1301–1311.
- Self W, Semler M, Bellomo R, et al. Liberal versus restrictive intravenous fluid therapy for early septic shock: rationale for a randomized trial. Ann Emerg Med. 2018;72:457-466.
- Motzkus CA, Lilly CM. Accountability for sepsis treatment: the SEP-1 Core Measure. Chest. 2017;151:955-957.
- Marik P. Guest post: iSepsis – death by fluids, part 1. EMCrit RACC. https://emcrit.org/emcrit/isepsis-death-fluids-part-1. Published September 30, 2017. Accessed October 31, 2021.
- Marik P. Guest post: iSepsis – death by fluids, part 2. EMCrit RACC. https://emcrit.org/emcrit/isepsis-death-fluids-part-2. Published October 15, 2017. Accessed October 31, 2021.
- Marik P. Guest post: iSepsis – death by fluids, part 3. EMCrit RACC. https://emcrit.org/emcrit/isepsis-death-fluid-part-3. Published October 28, 2017. Accessed October 31, 2021.
- Marik P. Guest post: iSepsis – death by fluids, part 4. EMCrit RACC. https://emcrit.org/emcrit/isepsis-death-fluids-part-4. Published December 10, 2017. Accessed October 31, 2021.
- Mackenzie D. Resus of the hypotensive patient part 1 – when IV fluids kill. Downeast Emergency Medicine.https://www.downeastem.org/downeastem/2018/1/15/when-iv-fluids-kill. Published January 16, 2018. Accessed October 31, 2021.
- Mackenzie D. Resus of the hypotensive patient part 2 – why you should be using peripheral pressors (and not feeling guilty about it). Downeast Emergency Medicine.https://www.downeastem.org/downeastem/2018/1/15/when-iv-fluids-kill-brxpt. Published January 23, 2018. Accessed October 31, 2021.
- Evans L, Rhodes A, Alhazzani W, et al. Surviving Sepsis Campaign: international guidelines for management of sepsis and septic shock 2021. Care Med. 2021;49(11):1-81.





